
Gastroenterology (Y2)
Question 1: Which of the following best describes the Rome IV criteria for diagnosing functional constipation?
A) Symptoms must be present for at least 3 months, with onset 6 months prior, and include infrequent bowel movements (<3 per week).
B) Symptoms must be present for 6 months, with infrequent diarrhoea and alternating constipation.
C) Symptoms must include blood in stool and weight loss.
D) Symptoms must include abdominal pain relieved by defecation.
E) Symptoms must include nausea and vomiting with infrequent bowel movements.
Question 2: What is the mechanism of action of alginates in treating reflux symptoms?
A) They neutralize gastric acid.
B) They form a physical barrier to prevent reflux.
C) They reduce gastric acid secretion.
D) They increase gastric motility.
E) They block histamine receptors in the stomach.
Question 3: Which of the following best describes a Billroth II procedure?
A) Partial gastrectomy with anastomosis to the duodenum.
B) Total gastrectomy with oesophagojejunostomy.
C) Subtotal gastrectomy with ileal bypass.
D) Right hemicolectomy.
E) Partial gastrectomy with gastrojejunostomy.
Question 4: A patient presents with dizziness, sweating, and diarrhoea 30 minutes after eating. What is the most likely diagnosis?
A) Postprandial hypoglycaemia
B) Dumping syndrome
C) Gastroparesis
D) Reactive hypoglycaemia
E) Bile acid malabsorption
Question 5: A 50-year-old male undergoes a RYGB. On postoperative day 3, he develops fever, tachycardia, and generalised abdominal pain. What is the most likely diagnosis?
A) Dumping syndrome
B) Small bowel obstruction
C) Anastomotic leak
D) Wound infection
E) Postoperative ileus
Question 6: A patient with chronic bloating, abdominal pain, and intermittent diarrhoea notices that symptoms improve after following a special diet. What does this diet primarily restrict?
A) High-fat foods
B) High-protein foods
C) Foods high in gluten
D) Foods containing fermentable oligosaccharides, disaccharides, monosaccharides, and polyols
E) Foods high in lactose
Question 7: A 34-year-old woman presents with chronic diarrhoea after eating bread, bloating and abdominal pain. Blood tests reveal iron-deficiency anaemia, and serology shows elevated anti-tissue transglutaminase (tTG) IgA levels. What is the most likely diagnosis?
A) Irritable Bowel Syndrome (IBS)
B) Crohn’s Disease
C) Coeliac Disease
D) Lactose Intolerance
E) Microscopic colitis
Question 8: A 58-year-old woman presents with chronic, non-bloody watery diarrhoea for six months. She denies abdominal pain, weight loss, or systemic symptoms. Colonoscopy reveals a normal mucosal appearance, but biopsy shows subepithelial collagen deposition and lymphocytic infiltration. What is the most likely diagnosis?
A) Crohn’s Disease
B) Irritable Bowel Syndrome (IBS)
C) Ulcerative Colitis
D) Microscopic Colitis
E) Coeliac Disease
Question 9: A 45-year-old man presents with epigastric pain, nausea, and bloating. He has a history of frequent use of nonsteroidal anti-inflammatory drugs (NSAIDs) for joint pain. He also reports occasional vomiting and has noticed black stools. What is the most likely diagnosis?
A) Peptic Ulcer Disease (PUD)
B) Gastroesophageal Reflux Disease (GERD)
C) Helicobacter pylori Infection
D) Gastric cancer
E) Celiac Disease
Question 10: A newborn is diagnosed with a congenital abdominal wall defect where the intestines protrude through a hole beside the umbilical cord. The defect is not covered by a sac. What is the most likely diagnosis?
A) Omphalocele
B) Gastroschisis
C) Umbilical Hernia
D) Diaphragmatic Hernia
E) Meckel’s Diverticulum
Question 11: Which of the following is the primary cause of hepatic encephalopathy (HE)?
A) Elevated bilirubin levels
B) Accumulation of ammonia in the bloodstream
C) Portal hypertension
D) Increased protein synthesis by the liver
E) Obstruction of bile flow
Question 12: How does ascites develop in cirrhosis?
A) Decreased ammonia clearance
B) Increased bile production
C) Portal hypertension and hypoalbuminemia
D) Excessive protein intake
E) Obstruction of bile flow
Question 13: What distinguishes hepatopulmonary syndrome (HPS) from portopulmonary hypertension (PPH)?
A) HPS involves increased pulmonary vascular resistance, while PPH involves intrapulmonary vasodilation.
B) HPS occurs in acute liver failure, while PPH occurs in chronic liver disease.
C) HPS is caused by bile accumulation, while PPH is caused by ammonia buildup.
D) HPS is reversible, while PPH is irreversible.
E) HPS involves intrapulmonary vasodilation and hypoxemia, while PPH involves pulmonary artery hypertension.
Question 14: Which of the following is the most specific diagnostic feature of acute pancreatitis?
A) Elevated serum bilirubin
B) Abdominal ultrasound showing gallstones
C) Jaundice
D) Serum amylase/lipase >3 times the upper limit of normal
E) Steatorrhea
Question 15: A 48-year-old male presents with severe upper abdominal pain radiating to the back, nausea, and vomiting. His lipase level is 5 times the upper limit of normal. What is the most appropriate initial treatment?
A) Start broad-spectrum antibiotics
B) Administer IV crystalloid fluids (Ringer’s lactate)
C) Perform an immediate ERCP
D) Schedule an emergency Kausch-Whipple resection
E) Begin pancreatic enzyme replacement therapy
Question 16: Which of the following is a common feature of chronic pancreatitis?
A) Intermittent or continuous upper abdominal pain
B) Persistent jaundice
C) Serum amylase/lipase >3 times the upper limit of normal
D) Acute organ failure
E) Hyperglycaemia in the absence of malabsorption
Question 17: Which of the following is the most significant risk factor for the development of oesophageal squamous cell carcinoma?
A) Chronic gastroesophageal reflux disease (GORD)
B) Helicobacter pylori infection
C) Smoking and alcohol consumption
D) Low-grade squamous dysplasia
E) Barrett’s oesophagus
Question 18: Which of the following gastric cancers is most likely to arise in the context of Helicobacter pylori infection?
A) Diffuse type adenocarcinoma
B) Gastric lymphoma
C) Gastrointestinal stromal tumour (GIST)
D) Neuroendocrine tumour
E) Intestinal type adenocarcinoma
Question 19: Which type of colonic adenoma has the highest risk of malignant transformation?
A) Tubular adenoma with low-grade dysplasia
B) Tubulovillous adenoma with high-grade dysplasia
C) Metaplastic polyp
D) Villous adenoma
E) Hyperplastic polyp
Question 20: Which of the following syndromes is most associated with microsatellite instability and mutations in DNA mismatch repair genes?
A) Familial adenomatous polyposis (FAP)
B) Hereditary non-polyposis colorectal cancer (HNPCC)
C) Peutz-Jeghers syndrome
D) Lynch syndrome
E) Juvenile polyposis syndrome
Question 21: Which of the following populations is most vulnerable to severe dehydration from astrovirus infection?
A) Young children
B) Elderly individuals
C) Pregnant women
D) B and C
E) A and B
Question 22: Which of the following is the most common cause of viral gastroenteritis in all age groups worldwide?
A) Norovirus
B) E-coli
C) Rotavirus
D) Adenovirus
E) Rhinovirus
Question 23: Which pathogen is most likely to cause watery diarrhoea after consuming fried rice?
A) Yersinia enterocolitica
B) Vibrio cholerae
C) Shigella
D) Bacillus cereus
E) Clostridium perfringens
Question 24: A pregnant woman consumes unpasteurised cheese and develops fever, muscle aches, and mild diarrhoea. What is the most likely pathogen?
A) Salmonella
B) Campylobacter jejuni
C) Listeria monocytogenes
D) Vibrio cholerae
E) Clostridium perfringens
Question 25: A 10-year-old boy presents with periumbilical pain that migrates to the right lower quadrant, accompanied by nausea and fever. On examination, there is tenderness at McBurney’s point and rebound tenderness. What is the initial pathological event in the development of appendicitis?
A) Bacterial overgrowth
B) Luminal obstruction
C) Ischemia of the appendix wall
D) Perforation of the appendix
E) Necrosis of the appendix
Question 26: A 45-year-old man with ulcerative colitis presents with jaundice, pruritus, and fatigue. Imaging reveals beading of the bile ducts, and liver biopsy shows concentric fibrosis around bile ducts. What is the most likely diagnosis?
A) Primary Biliary Cholangitis (PBC)
B) Autoimmune hepatitis
C) Alcoholic hepatitis
D) Wilson’s disease
E) Primary Sclerosing Cholangitis (PSC)
Question 27: A 34-year-old woman presents with recurrent episodes of abdominal pain particularly in the lower left quadrant, bloating, and diarrhoea. She has noticed blood mixed with her stool during some episodes. On plain film, the colon seems to lack haustra. What is the most likely diagnosis?
A) Crohn’s Disease
B) Irritable Bowel Syndrome (IBS)
C) Ulcerative Colitis
D) Microscopic Colitis
E) Coeliac Disease
Question 28: A 70-year-old man presents with acute left lower quadrant abdominal pain, fever, and constipation. A CT scan shows thickening of the sigmoid colon and peri colonic fat stranding. What is the most likely diagnosis?
A) Diverticulitis
B) Diverticulosis
C) Colorectal Cancer
D) IBS
E) Inflammatory Bowel Disease (IBD)
Question 29: What radiological sign is this associated with?
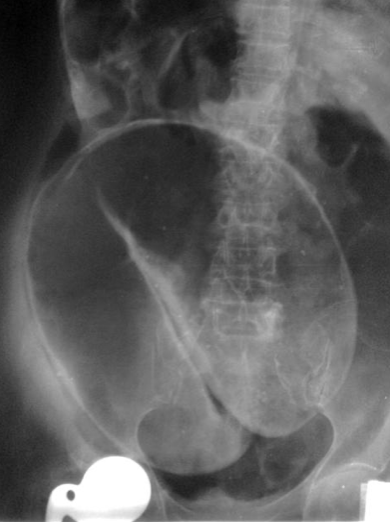
A) Colitis
B) Pneumoperitoneum
C) Caecal volvulus
D) Sigmoid volvulus
E) Small bowel obstruction
Question 30: A 28-year-old man presents with chronic diarrhoea, abdominal pain, and weight loss. Blood tests reveal mild anaemia and an elevated C-reactive protein (CRP). Stool testing shows significantly elevated faecal calprotectin. Colonoscopy reveals patchy inflammation with cobble stoning and skip lesions. Which of the following tests is most specific for confirming inflammatory bowel disease (IBD)?
A) Complete Blood Count (CBC)
B) Faecal Calprotectin
C) Colonoscopy with Biopsy
D) C-Reactive Protein (CRP)
E) Stool Culture
Question 31: A 35-year-old patient presents with difficulty distinguishing tastes on the anterior and posterior parts of their tongue. Upon examination, you notice reduced sensation and taste perception in different regions. Based on the sensory innervation of the tongue, which of the following statements is most accurate regarding the innervation of the tongue?
A) The anterior 1/3 of the tongue receives both general and taste sensation through the glossopharyngeal nerve.
B) The posterior 1/3 of the tongue receives general sensation from the lingual nerve and taste sensation from the chorda tympani.
C) The anterior 1/3 of the tongue receives general sensation from the lingual nerve (CN V3) and taste sensation from the chorda tympani (CN VII).
D) The posterior 1/3 of the tongue receives both general and taste sensation through the lingual nerve.
E) The posterior 1/3 of the tongue receives general sensation from the glossopharyngeal nerve and taste sensation from the vagus nerve.
Question 32: A 47-year-old male presents with persistent heartburn, regurgitation, and difficulty swallowing over the past several months. He reports that his symptoms worsen at night and he frequently experiences a sour taste in his mouth. He has a history of smoking and consumes alcohol regularly. The physician suspects gastro-oesophageal reflux disease (GORD). Which of the following statements about the pathophysiology and management of gastro-oesophageal reflux disease (GORD) is correct?
A) GORD is primarily caused by an abnormal relaxation of the lower oesophageal sphincter (LOS) and can be exacerbated by obesity, smoking, and alcohol consumption.
B) Proton pump inhibitors (PPIs) are not effective in treating GORD-related symptoms since they do not alter the acid levels in the oesophagus.
C) GORD is only diagnosed through esophagogastroduodenoscopy (OGD) when symptoms persist for more than 6 months.
D) Lifestyle modifications, such as weight loss and elevating the head of the bed, are not considered essential in managing GORD symptoms.
E) Barrett’s oesophagus is a benign condition that does not increase the risk of oesophageal adenocarcinoma, even with prolonged acid exposure.
Question 33: A 63-year-old male presents with persistent epigastric pain, unintentional weight loss over the past few months, and early satiety. He reports having occasional vomiting and a history of chronic dyspepsia. He has also noted some black stools recently. His family history includes a relative with a gastric carcinoma. Which of the following is the most appropriate next step in the diagnosis and management of this patient?
A) Treat empirically for peptic ulcer disease (PUD) with proton pump inhibitors (PPIs) and H. pylori eradication therapy, with follow-up in 6-8 weeks.
B) Start immediate chemotherapy to manage potential gastric cancer, as it is poorly responsive to surgery.
C) Perform an esophagogastroduodenoscopy (OGD) to evaluate for peptic ulcer disease, excluding malignancy and obtaining a biopsy for histological confirmation.
D) Order a barium swallow to assess for gastric outlet obstruction, as this is more likely than gastric cancer.
E) Refer the patient to surgery immediately to remove the tumour, as gastric cancer can be effectively treated with surgery without further investigations.
Question 34: A 40-year-old male with a history of recurrent peptic ulcers presents with symptoms including diarrhoea, abdominal pain, and unintentional weight loss. Further testing reveals a markedly elevated serum gastrin level. He has a family history of endocrine disorders. Based on the pathophysiology of this condition, which of the following mutations or mechanisms is most likely responsible for this patient’s symptoms?
A) A mutation in the MEN1 gene, which results in the development of multiple endocrine neoplasia type I, leading to the formation of a Zollinger Ellison Syndrome.
B) Overexpression of the CagA protein by Helicobacter pylori, causing gastric metaplasia and hypergastrinemia.
C) Autoimmune destruction of parietal cells, leading to decreased intrinsic factor and B12 deficiency, which stimulates excess gastrin production.
D) Mutations in the APC gene, resulting in the formation of gastric adenomas that secrete excessive amounts of gastrin.
E) An upregulation of the SSTR2 receptor, leading to excessive secretion of somatostatin and subsequent hypergastrinemia.
Question 35: A 45-year-old male with a history of dyspepsia presents to the clinic. Based on the clinical symptoms and suspicion of Helicobacter pylori infection, the physician is considering testing to confirm the diagnosis. Which of the following non-invasive tests for H. pylori detection would be the most appropriate first-line approach for this patient?
A) 13C-urea breath test, as it is a non-invasive test that directly detects the presence of active H. pylori infection.
B) Faecal antigen test, which is highly specific and should be used only after a positive breath test.
C) Serology (IgG), as it is a non-invasive test that detects past or current infection but may not distinguish active infection.
D) Rapid urease test on gastric biopsy, as it provides a definitive diagnosis but requires invasive endoscopy.
E) Combination of two antibiotics (Amoxicillin + Clarithromycin) and a proton pump inhibitor (PPI), which should be used immediately as part of the diagnostic process.
Question 36: A 28-year-old female presents with chronic diarrhoea, bloating, and unexplained weight loss. Laboratory tests reveal iron-deficiency anaemia. On physical examination, she has a vesicular, itchy rash consistent with dermatitis herpetiformis. Based on her clinical presentation, the physician suspects coeliac disease. Which of the following most accurately describes the pathophysiology of coeliac disease?
A) Coeliac disease is primarily caused by a hypersensitivity reaction to gluten, involving IgE antibodies against gliadin, leading to direct mast cell degranulation and intestinal inflammation.
B) In coeliac disease, gliadin, a component of gluten, triggers an immune response that leads to the production of IgA antibodies against both gliadin and transglutaminase, resulting in tissue damage.
C) Coeliac disease is a result of a viral infection, such as rotavirus, which leads to inflammation of the gut and loss of microvilli.
D) The immune response in coeliac disease is directed against the HLA-DQ2/DQ8 receptors, causing direct damage to the small intestine epithelial cells.
E) In coeliac disease, a deficiency of vitamin D leads to damage of the villi, resulting in gastrointestinal symptoms and anaemia.
Question 37: A 34-year-old female with a history of irritable bowel syndrome (IBS) presents with bloating, excessive gas, and abdominal discomfort, which are exacerbated after meals. Her physician suggests trying a ‘specific’ diet to reduce her symptoms. This specific diet involves the elimination of food that are known to cause increased gas production and luminal distension. Which of the following food groups should be avoided whilst on this diet due to their potential to ferment in the bowel, leading to gas production and abdominal distension?
A) Foods high in protein, such as meat and eggs, as they contribute to gut inflammation and bloating.
B) Foods containing high levels of fructose, lactose, oligosaccharides, and polyols, as these ferment in the bowel and cause luminal distension.
C) High-fibre foods such as whole grains and legumes, which directly affect gut motility but not gas production.
D) High-fat foods, such as butter and oils, which slow down digestion and contribute to bloating.
E) Foods rich in soluble fibre, such as oats and beans, which can lead to excess water retention in the gut.
Question 38: A 55-year-old male with advanced colorectal cancer presents with worsening abdominal pain and distension. A CT scan reveals fluid accumulation in the abdominal cavity. The physician is concerned about the potential spread of infection and tumour through the peritoneal spaces. Based on your knowledge of peritoneal fluid circulation and anatomical spaces, which of the following best describes how peritoneal fluid can facilitate the spread of infection or tumour from the pelvis to the upper abdomen?
A) Fluid from the pelvis drains into the left sub-phrenic space via the gastro-hepatic ligament.
B) The left sub-hepatic space is continuous with the right para-colic space, allowing for disease spread across both sides of the abdomen.
C) Fluid from the pelvis drains into the right para-colic space and subsequently ascends into the right sub-phrenic space.
D) Morrison’s Pouch, being the most dependent part of the abdomen, prevents the spread of infection from the sub-hepatic space.
E) Peritoneal fluid primarily accumulates in the paracolic gutters, but it does not contribute to disease spread to the sub-phrenic spaces.
Question 39: A 2-year-old male presents with acute lower abdominal pain, vomiting, and bloody stools. The symptoms are similar to appendicitis, and the child is taken for imaging studies. The imaging reveals a small outpouching of the ileum that appears to have gastric mucosa. Which of the following statements best describes the pathophysiology and clinical features of Meckel’s Diverticulum?
A) Meckel’s Diverticulum occurs due to an abnormality in the development of the abdominal wall, leading to a para-umbilical herniation of the small bowel without any membrane surrounding it.
B) Meckel’s Diverticulum is a congenital defect of the intestinal vasculature that leads to malrotation of the bowel, often presenting with large abdominal distension and vomiting.
C) Meckel’s Diverticulum is associated with omphalocele, where the intestines and liver protrude out of the umbilicus, still covered by the peritoneal membrane, and requires immediate surgical repair after birth.
D) Meckel’s Diverticulum is most associated with gastroschisis, where the bowel herniates through a para-umbilical defect, presenting as a free-floating mass with no covering membrane and requiring surgical intervention.
E) Meckel’s Diverticulum is a failure of the vitellointestinal duct to close, leading to persistent communication between the yolk sac and the midgut, which may cause bleeding, pain, and mimic appendicitis.
Question 40: A 32-week pregnant woman undergoes an antenatal ultrasound scan, which reveals a defect in the abdominal wall of the foetus. The scan shows loops of bowel herniating to the right of the umbilicus with no covering membrane. Which of the following best describes the key difference between gastroschisis and omphalocele?
A) Gastroschisis involves a herniation of bowel loops through a para-umbilical defect with no surrounding membrane, whereas omphalocele involves herniated intestines (and sometimes other organs) covered by the peritoneal membrane and amnion.
B) In omphalocele, the defect is located to the right of the umbilicus, while gastroschisis is located directly through the umbilicus.
C) Omphalocele occurs due to genetic and environmental factors leading to compromised vasculature in the abdominal wall, whereas gastroschisis results from failure of the intestines to return to the abdomen after natural protrusion during foetal development.
D) Omphalocele is a defect of the abdominal wall in which the intestines are free-floating, while gastroschisis is a condition where the intestines are still attached to the peritoneal membrane.
E) Gastroschisis occurs when the intestines are herniated through the umbilical cord, while omphalocele involves a midline defect of the abdominal wall.
Question 41: A 30-year-old woman presents with chronic abdominal pain, intermittent diarrhoea, and recent weight loss. She has a history of smoking and is currently taking an oral contraceptive. Her symptoms have been ongoing for several months, and she reports occasional fistula formation. A colonoscopy reveals transmural inflammation, and biopsy confirms granulomas in the affected areas. Which of the following statements accurately contrasts Crohn’s Disease with Ulcerative Colitis?
A) Crohn’s Disease is characterised by superficial inflammation confined to the sigmoid colon, while Ulcerative Colitis involves transmural inflammation affecting the entire GI tract.
B) In Crohn’s Disease, there is often a singular phase of severe activity followed by intermittent flare-ups, while Ulcerative Colitis presents with progressively worsening ulcers that spread throughout the GI tract.
C) Both Crohn’s Disease and Ulcerative Colitis are managed primarily with surgery, but while surgery is often curative in Ulcerative Colitis, it is rarely curative in Crohn’s Disease due to its nature of progressive ulceration and involvement of multiple GI tract areas.
D) In Crohn’s Disease, strictures and fistulas are common due to transmural inflammation, while in Ulcerative Colitis, superficial inflammation leads to blood in the stool, urgency, and tenesmus, but strictures and fistulas are rare.
E) Ulcerative Colitis is more likely to be associated with fistula formation and weight loss than Crohn’s Disease, where weight loss is less frequent, and fistulas are uncommon.
Question 42: A 65-year-old woman presents with complaints of involuntary loss of faeces and flatulence for the past few months. She describes episodes in which she is aware of the need to defecate but is unable to reach the toilet in time. She also reports occasional leakage of gas. On examination, she has a history of a forceps delivery during childbirth and some perineal numbness. She is currently being treated for diabetes mellitus. Which of the following is the most likely underlying cause of this patient’s faecal incontinence?
A) Overflow incontinence due to diabetes-induced rectal hypomotility, leading to faecal retention and eventual leakage.
B) Decreased rectal compliance from chronic proctitis, resulting in an inability to store faeces and causing urge incontinence.
C) Neurological damage from pudendal nerve trauma during childbirth, leading to anal sphincter weakness and decreased rectal sensation.
D) Passive incontinence due to diabetes mellitus, resulting in complete loss of sensation to the rectum, leading to involuntary stool loss without prior awareness.
E) Idiopathic incontinence, possibly related to an undiagnosed sacral nerve injury, causing sphincter weakness and decreased perception of rectal sensation.
Question 43: A 55-year-old woman presents to the clinic with episodes of nausea, weakness, and dizziness occurring shortly after eating large meals. She describes a feeling of fullness, followed by abdominal cramping and diarrhoea. She also experiences light-headedness and rapid heart rate shortly after eating. The patient had undergone partial gastrectomy with jejunal reconstruction for peptic ulcer disease 6 months ago. Which of the following is the most likely explanation for her symptoms?
A) Excessive secretion of insulin after meals causing postprandial hypoglycaemia and flushing.
B) Increased gastric acid secretion leading to irritation of the stomach lining and postprandial discomfort.
C) Small bowel bacterial overgrowth leading to malabsorption and bloating after meals.
D) Pancreatic insufficiency leading to unabsorbed fats causing nausea and diarrhoea postprandially.
E) Rapid gastric emptying causing an osmotic load that leads to fluid shifts into the small bowel.
Question 44: A 48-year-old woman presents with chronic watery diarrhoea that has persisted for the past two months. She reports that despite her symptoms, her colonic appearance on colonoscopy was normal. Her past medical history includes rheumatoid arthritis, and she is currently taking ibuprofen daily for joint pain. A biopsy of her colon shows histological inflammation but no significant thickening of the subepithelial collagen table. What is the most likely underlying mechanism causing this patient’s symptoms?
A) Increased gastric acid secretion leading to irritation and malabsorption in the colon.
B) Increased permeability of the colon allowing luminal antigens to promote inflammation, impairing sodium and chloride absorption.
C) Chronic use of proton pump inhibitors leading to small bowel bacterial overgrowth and malabsorption.
D) Autoimmune-mediated destruction of the enteric nervous system, leading to impaired motility.
E) Impaired absorption of bile acids resulting in osmotic diarrhoea.
Question 45: A 35-year-old man presents with severe abdominal pain, vomiting, and watery diarrhoea following a buffet meal at a local restaurant. His symptoms began within a few hours after eating, and he is otherwise healthy. He reports no history of recent travel or contact with animals. On examination, he has no fever or significant dehydration. Based on the pathogen’s association and clinical presentation, which of the following is the most likely causative agent?
A) Vibrio cholerae
B) Bacillus cereus
C) Yersinia enterocolitica
D) Campylobacter jejuni
E) Salmonella (non-typhoidal)
Question 46: A 40-year-old woman presents with severe crampy abdominal pain, fever, and bloody diarrhoea that began 24 hours after attending a family picnic. She reports consuming undercooked chicken and a salad containing raw vegetables. On examination, she has abdominal tenderness, particularly in the lower abdomen. Her white blood cell count is elevated, and stool cultures are ordered. Based on the clinical presentation and potential pathogens, which of the following is the most likely causative agent?
A) Shigella dysenteriae
B) Escherichia coli O157:H7
C) Clostridium difficile
D) Listeria monocytogenes
E) Giardia lamblia
Question 47: A 4-year-old child and a 65-year-old elderly patient both present with symptoms of gastroenteritis, including vomiting and diarrhoea. The child was not fully vaccinated for rotavirus, and the elderly patient recently experienced exposure in a nursing home setting. Based on their age and typical clinical features, how would the presentation of these two viruses most likely differ between the child and the elderly patient?
A) The child is more likely to experience severe dehydration and a longer duration of diarrhoea, while the elderly patient is more likely to have a sudden onset of vomiting and diarrhoea that lasts for a shorter period.
B) The child will have mild, non-severe symptoms with no dehydration, whereas the elderly patient will experience severe vomiting and cramping that may last up to a week.
C) Both the child and elderly patient are likely to experience similar symptoms, but the child will have more severe vomiting and the elderly patient will present with mild diarrhoea.
D) The child is likely to experience more severe vomiting, while the elderly patient will have more severe diarrhoea and a prolonged illness.
E) The elderly patient is more likely to have vomiting and diarrhoea that resolves in 24 to 48 hours, while the child will experience persistent vomiting with little improvement.
Question 48: A 55-year-old patient undergoes a routine colonoscopy, revealing three colonic polyps:
- A 1.5 cm tubular adenoma in the sigmoid colon.
- A 0.8 cm tubulo-villous adenoma in the descending colon.
- A 1.4 cm villous adenoma in the rectum.
Which of the following best describes the relative malignant potential of these polyps based on their histological type and size?
A) The tubular adenoma has the highest malignant potential due to its prevalence in the colon.
B) The tubulo-villous adenoma has negligible malignant potential compared to the other types.
C) Villous adenomas confer the highest malignant potential, especially when larger than 2 cm.
D) Tubular adenomas and villous adenomas carry equivalent malignant potential, as size is the only factor that determines malignancy.
E) Tubulo-villous adenomas carry the highest malignant potential regardless of size or type.
Question 49: A 45-year-old man with a strong family history of colorectal cancer is found to have a right-sided colon mass. Genetic testing reveals a mutation in one of his DNA mismatch repair (MMR) genes, and further history reveals a family member with endometrial cancer. Another patient, a 30-year-old woman, is diagnosed with hundreds of adenomatous polyps scattered throughout her colon on colonoscopy. Her genetic testing shows an APC gene mutation. Which of the following statements accurately compares the genetic basis and features of these two inherited colorectal cancer syndromes?
A) Both conditions involve mutations in DNA mismatch repair genes leading to microsatellite instability.
B) Familial Adenomatous Polyposis (FAP) is more commonly associated with extra-colonic cancers like endometrial and ovarian cancer than Lynch Syndrome.
C) Lynch Syndrome is caused by mutations in APC, which leads to the development of numerous adenomatous polyps throughout the colon.
D) FAP is caused by mutations in the APC tumour suppressor gene, while Lynch Syndrome involves mutations in DNA mismatch repair genes such as MLH1 and MSH2.
E) Both conditions present with polyposis of the colon, but FAP is associated with a higher overall cancer risk than Lynch Syndrome.
Question 50: A 55-year-old patient undergoes surgical excision of a suspicious mass. The pathology report describes the mass as “well-circumscribed, encapsulated, and homogenous on cut-surface.” Microscopic examination reveals no evidence of invasion, although the tumour shows some pleomorphism and moderate differentiation. Which of the following features would most reliably distinguish this neoplasm from a malignant tumour?
A) Presence of pleomorphism in the cells of the tumour
B) The tumour has a homogenous cut-surface on macroscopic examination
C) Evidence of a high mitotic index on microscopic examination
D) Encapsulation and lack of invasion in the surrounding tissue
E) Increased cytoplasmic-to-nuclear ratio in the tumour cells
Question 51: A 62-year-old patient presents with vague abdominal discomfort and early satiety. After endoscopy, a biopsy reveals adenocarcinoma of the stomach. Histological examination shows poorly cohesive malignant cells with signet-ring morphology, and macroscopically, the stomach wall appears thickened and leather-like. Based on the findings, which of the following features best describes this patient’s condition?
A) Well-localised, infiltrative carcinoma with a better prognosis
B) Glandular dysplasia without evidence of malignant invasion
C) A diffuse infiltration of poorly cohesive cancer cells with a poor prognosis
D) Presence of intestinal metaplasia without significant clinical consequences
E) A solitary polyp-like lesion confined to the mucosal layer
Question 52: A 58-year-old woman presents with symptoms of weight loss, recurrent abdominal pain, and severe peptic ulcers that do not respond to standard proton pump inhibitor therapy. Laboratory results show elevated levels of gastrin. Endoscopic examination reveals multiple gastric ulcers, and a biopsy indicates a neuroendocrine tumour. Which of the following best explains the pathophysiology of the tumour in this patient?
A) A mutation in the APC gene leading to uncontrolled cell division
B) Chronic inflammation of the gastric mucosa stimulating increased acid production by parietal cells
C) G-cells in the antrum producing excessive gastrin in response to low stomach acid levels
D) Destruction of the parietal cells leading to gastrin overproduction by ECL cells
E) Genetic mutations in mesenchymal cells leading to the formation of a stromal tumour
Question 53: A 45-year-old male presents with severe upper abdominal pain radiating to the back, nausea, and vomiting. He has a history of heavy alcohol consumption. Blood tests reveal serum amylase and lipase levels three times the normal limit. A CT scan shows pancreatic enlargement without any clear signs of necrosis or fluid collections. Which of the following is the most likely diagnosis, and what is the underlying pathophysiological mechanism?
A) Acute pancreatitis due to gallstones, caused by retrograde bile duct obstruction
B) Acute pancreatitis due to alcohol consumption, leading to the activation of pancreatic enzymes
C) Chronic pancreatitis due to long-term alcohol use, causing irreversible damage
D) Pancreatic carcinoma, leading to obstructive symptoms and enzyme elevation
E) Acute cholecystitis, resulting in bile duct obstruction and enzyme elevation
Question 54: A 62-year-old male is participating in the National Bowel Cancer Screening programme in the UK. He has been sent a stool sample kit, which detects faecal occult blood (FOB). The test returns a positive result, and he is now being referred for further investigation with flexible sigmoidoscopy. Which of the following is true regarding the screening programme and its limitations?
A) The FOB test is highly sensitive, with very few false positives
B) The current stool sample test (FOB) has poor specificity so is being replaced by a test that detects FIT blood
C) The flexible sigmoidoscopy is part of the Bowel Scope programme, which is for individuals over 55 years old
D) The FIT test, which will replace the FOB test, has reduced sensitivity but higher specificity
E) The Bowel Scope programme is aimed at reducing CRC incidence and mortality by using stool samples every 2 years
Question 55: A 35-year-old male with a history of heavy alcohol consumption presents to the clinic with complaints of fatigue, dehydration, and a general feeling of malaise after binge drinking the previous night. He has elevated liver enzymes and his blood ethanol level is found to be significantly higher than what would be expected from the typical metabolic process. Which of the following mechanisms is most likely contributing to the faster metabolism of alcohol in this patient?
A) Increased activity of Alcohol Dehydrogenase (ADH) and Mitochondrial Acetaldehyde Dehydrogenase (ALDH)
B) Induction of the microsomal ethanol oxidising system (MEOS) by chronic alcohol use
C) Decreased NADH production leading to reduced oxidative phosphorylation
D) Reduced activity of Cytochrome P450IIE1 due to chronic drinking
E) Inhibition of alcohol metabolism by high blood acetate levels
Question 56: A 40-year-old male presents with jaundice, fatigue, and mild upper abdominal discomfort. He has a history of intravenous drug use and recently travelled to Southeast Asia. His liver function tests reveal elevated ALT and AST levels, and a liver ultrasound shows mild hepatomegaly. He is otherwise healthy, with no known history of chronic liver disease. Which of the following best describes the likely diagnosis and the course of the infection in this patient?
A) The patient is likely infected with Hepatitis B, and while he may experience an acute infection, he is at risk of developing chronic liver disease and should be monitored for cirrhosis.
B) The most likely infection is Hepatitis C, which can lead to a chronic infection in 80% of cases, with a risk of cirrhosis and hepatocellular carcinoma over time.
C) This patient likely has Hepatitis E, which will be self-limiting and should resolve without long-term complications.
D) The infection is most likely Hepatitis D, which is dependent on co-infection with Hepatitis B and could worsen the patient’s condition if both infections are present.
E) Hepatitis A is the most probable diagnosis, and while self-limiting, the patient should avoid alcohol to prevent further liver damage during recovery.
Question 57: A 55-year-old male with a long history of heavy alcohol use presents to the clinic with complaints of fatigue, weight loss, and mild abdominal distension. On examination, he is noted to have jaundice, spider angiomas, and an enlarged, firm liver. Laboratory findings show elevated liver enzymes (AST and ALT), elevated bilirubin, and a low albumin level. An ultrasound reveals moderate ascites. Based on his clinical presentation and lab results, which of the following stages of cirrhosis is most likely for this patient?
A) Stage 0 – Mild portal hypertension without varices
B) Stage 1 – Compensated cirrhosis with clinically significant portal hypertension
C) Stage 2 – Compensated cirrhosis with varices but no decompensation
D) Stage 3 – Decompensated cirrhosis with bleeding complications
E) Stage 4 – Decompensated cirrhosis with first non-bleeding decompensation
Question 58: A 55-year-old woman with a history of chronic alcohol consumption presents to the emergency department with abdominal distension, shortness of breath, and fatigue. She also reports recent episodes of increased swelling in her legs and a decreased appetite. On examination, she is found to have jaundice, spider angiomas, palmar erythema, and ascites. Laboratory results show elevated bilirubin, low albumin, and increased prothrombin time. An abdominal ultrasound reveals hepatomegaly, ascites, and splenomegaly. Which of the following findings is most likely to be present in this patient due to her underlying condition?
A) Normal renal function
B) Hypoxemia with arterial oxygen desaturation
C) Increased platelet count
D) Elevated alkaline phosphatase (ALP)
E) Reduced sodium levels (hyponatremia)
Question 59: A 55-year-old woman presents with intermittent jaundice, right upper quadrant pain, and a history of chronic cholelithiasis. Recent imaging reveals a large stone in the gallbladder that has eroded through the gallbladder wall into the common bile duct. This condition is causing obstructive jaundice and cholangitis. What is the most likely diagnosis?
A) Mirizzi Syndrome
B) Gallbladder Carcinoma
C) Choledochal Cyst
D) Pancreatitis
E) Gallstone Ileus
Question 60: A 60-year-old male presents with jaundice and dark urine. On physical examination, he has a palpable mass in the right upper quadrant. His liver function tests reveal a raised conjugated bilirubin and an elevated alkaline phosphatase (ALP) level. Ultrasound reveals biliary duct dilation, but no stones are visible. What is the most likely next step in the investigation?
A) CT scan to evaluate for liver metastases or other structural abnormalities not visible on ultrasound.
B) Endoscopic Retrograde Cholangio-pancreatography (ERCP) to directly visualise the biliary tree and obtain biopsies if necessary.
C) MRI to assess for benign hepatic lesions and gallstones not visualised on ultrasound.
D) Endoscopic ultrasound to evaluate the biliary tree for strictures or other obstructions in the bile duct.
E) Perform a liver biopsy to confirm the presence of hepatic fibrosis or cirrhosis.
