
Neurology (Y2)
Question 1: A newborn has a small defect in the spine, but no visible bump or cyst. What type of spina bifida does this describe?
A. Spina bifida occulta
B. Spina bifida cystica
C. Encephalocele
D. Meningocele
E. Duane’s syndrome
Question 2: A 5-year-old girl presents with difficulty moving her left eye outward. Examination reveals that her sixth cranial nerve is underdeveloped. Which condition is most likely?
A. Amblyopia
B. Duane’s syndrome
C. strabismus
D. Cortical heterotopia
E. Syringomyelia
Question 3: Which zone of the developing brain is primarily responsible for generating new neurons during embryonic development?
A) Marginal Zone
B) Intermediate Zone
C) Subventricular Zone
D) Ventricular Zone
E) Cortical Plate
Question 4: A patient experiences seizures originating from one specific area of the brain, with no identifiable structural abnormality on imaging. What type of epilepsy is this likely to be?
A) Focal Epilepsy
B) Generalized Epilepsy
C) Cryptogenic Epilepsy
D) Secondary Epilepsy
E) Idiopathic Epilepsy
Question 5: Which toxin prevents the release of acetylcholine at the neuromuscular junction and can cause paralysis?
A) Tetanus toxin
B) Botulinum toxin
C) Saxitoxin
D) Dendrotoxin
E) Curare
Question 6: Which of the following nerves is primarily responsible for the sensation of the cornea?
A) Optic nerve
B) Facial nerve
C) Trigeminal nerve
D) Oculomotor nerve
E) Abducens nerve
Question 7: Which of the following is NOT involved in the production and drainage of tears?
A) Lacrimal gland
B) Trigeminal nerve
C) Lacrimal puncta
D) Nasolacrimal duct
E) Vitreous humour
Question 8: Which of the following is a common variant of Chronic Inflammatory Demyelinating Polyneuropathy (CIDP)?
A) Multifocal Motor Neuropathy (MMN)
B) Diabetic neuropathy
C) Lewis-Sumner Syndrome
D) Guillain-Barré Syndrome
E) Myasthenia Gravis
Question 9: Which of the following is a common negative symptom of schizophrenia?
A) Hallucinations
B) Delusions
C) Insomnia
D) Euphoria
E) Apathy
Question 10: In cases of locked-in syndrome, which part of the brain is primarily affected?
A) Medulla
B) Pons
C) Cerebellum
D) Thalamus
E) Hippocampus
Question 11: What is Horner’s Syndrome?
A) A disorder that causes involuntary movements in the face
B) A neurological condition resulting in paralysis of facial muscles
C) A condition characterized by a combination of ptosis, miosis, and anhidrosis
D) An infection that primarily affects the respiratory system
E) A type of stroke affecting the brainstem
Question 12: In a patient with increased muscle tone and spasticity, which condition is likely?
A) Lower motor neuron lesion
B) Upper motor neuron lesion
C) Neuromuscular junction disorder
D) Peripheral neuropathy
E) Myopathy
Question 13: What is the primary function of the reticular formation?
A) Maintenance of consciousness and arousal
B) Regulation of heart rate
C) Control of muscle movement
D) Processing sensory information
E) Coordination of voluntary movements
Question 14: Which of the following is a common positive symptom of schizophrenia?
A) Apathy
B) Hallucinations
C) Withdrawal into self
D) Reduced motivation
E) Anhedonia
Question 15: In the context of anxiety disorders, which medication class is known for its short-term effectiveness but risk of addiction?
A) SSRIs
B) SNRIs (Serotonin-Norepinephrine Reuptake Inhibitors)
C) Antipsychotics
D) Beta-blockers
E) Benzodiazepines
Question 16: What is the typical finding in a patient with Lateral Medullary Syndrome (Wallenberg Syndrome)?
A) Hemiparesis on the contralateral side
B) Dysphagia and loss of pain/temperature sensation on the ipsilateral side of the face
C) Complete loss of consciousness
D) Quadriplegia
E) Inability to speak
Question 17: What is the main cause of hypercalcaemia in patients with prolonged immobility?
A) Increased dietary calcium intake
B) Hyperparathyroidism
C) Bone breakdown exceeding formation
D) Renal failure
E) Malignancy
Question 18: A 70-year-old male presents with dizziness, difficulty swallowing, and right-sided facial numbness. Imaging shows a lesion in the brainstem. Which syndrome is most likely affecting this patient?
A) Locked-in syndrome
B) Lateral Medullary Syndrome (Wallenberg syndrome)
C) Internuclear ophthalmoplegia
D) Spinal shock
E) Multiple sclerosis
Question 19: A patient presents with unilateral ptosis (drooping eyelid), miosis (constricted pupil), and anhidrosis (lack of sweating) on the same side. What is the most likely diagnosis?
A) Horner’s Syndrome
B) Oculomotor nerve palsy
C) Myasthenia gravis
D) Guillain-Barré syndrome
E) Brown-Séquard syndrome
Question 20: A 70-year-old patient is brought to the clinic with memory loss and difficulty concentrating. Imaging studies reveal the presence of amyloid plaques and tau tangles. Which of the following statements best describes the roles of beta-amyloid and tau in Alzheimer’s disease?
A) Beta-amyloid is considered the primary cause of Alzheimer’s disease, while tau plays no significant role in cognitive decline.
B) Aggregation of beta-amyloid and tau proteins is solely protective and prevents neuronal death.
C) Beta-amyloid is crucial in triggering the Alzheimer’s process, while tau is important for its progression.
D) Tau proteins are the main contributors to the onset of Alzheimer’s disease, and beta-amyloid is secondary.
E) The presence of amyloid plaques directly correlates with the severity of cognitive impairment in all Alzheimer’s patients.
Question 21: A 60-year-old man presents with personality changes, including inappropriate social behaviour and language difficulties. MRI reveals atrophy of the frontal and temporal lobes. Which of the following findings is most characteristic of Pick’s disease?
A) Widespread beta-amyloid plaques throughout the brain.
B) Tau-containing Pick bodies inside neurons.
C) A strong correlation between beta-amyloid levels and cognitive decline.
D) Lewy bodies, composed of alpha-synuclein, in the substantia nigra.
E) Normal brain MRI with no atrophy or protein deposits.
Question 22: A patient presents with difficulties in writing but has normal speech and comprehension. Damage to which area is most likely to be involved?
A) Broca’s area, controlling speech production.
B) Wernicke’s area, involved in language comprehension.
C) The occipital cortex, responsible for visual processing.
D) The angular gyrus, associated with reading.
E) Exner’s area, near the motor cortex for hand movement.
Question 23: A patient is brought to the emergency room in a comatose state after a traumatic brain injury. Which of the following neural systems is most likely affected, leading to a loss of consciousness?
A) The occipital cortex
B) The lower brainstem, responsible for respiration
C) The reticular formation and ascending monoamine pathways
D) The cerebellum
E) The basal ganglia
Question 24) A 45-year-old man is involved in a car accident and suffers a traumatic brain injury. Post-accident, he has altered pain perception and difficulty controlling his emotional responses to pain. Imaging reveals damage near the cerebral aqueduct. Where is the periaqueductal grey matter located?
A) Pons
B) Medulla
C) Limbic system
D) Midbrain
E) Basal ganglia
Question 25: Which of the following describes the primary risk associated with performing a lumbar puncture in non-communicating hydrocephalus?
A) Infection of the central nervous system
B) Bleeding from the puncture site
C) Brain herniation
D) Increased intracranial pressure
E) Permanent spinal cord damage
Question 26: What is the most likely cause of phantom limb pain after an amputation?
A) Disruption of peripheral nerve endings, leading to abnormal brain signal
B) Increased blood flow to the remaining limb
C)Inflammation at the amputation site
D) Bacterial infection in the amputation area
E) Muscle atrophy in the remaining limb
Question 27: A 25-year-old woman presents with ptosis, miosis, and anhidrosis on the right side of her face. She also complains of mild pain in the neck and shoulder. Which of the following is the most likely diagnosis?
A) Bell’s palsy
B) Trigeminal neuralgia
C) Myasthenia gravis
D) Cluster headache
E) Horner’s syndrome
Question 28: A 35-year-old male with a history of trauma to his wrist presents with burning pain, swelling, and changes in skin colour over the affected area. The pain is described as deep and burning, and it is worse with light touch. Which of the following is the most likely diagnosis?
A) Complex regional pain syndrome (Type I)
B) Carpal tunnel syndrome
C) Phantom limb pain
D) Radial nerve injury
E) Tendonitis
Question 29: A 60-year-old man presents with bradykinesia, resting tremor, and a shuffling gait. His wife reports he has become slower and stiffer over the past year. Which of the following pathological findings is most likely associated with his condition?
A) Beta-amyloid plaques in the cerebral cortex
B) Tau protein tangles in neurons
C) Alpha-synuclein Lewy bodies in the substantia nigra
D) Loss of Purkinje cells in the cerebellum
E) Demyelination of motor neurons in the spinal cord
Question 30: Which of the following is most associated with chronic hypertension and affects deep brain structures like the basal ganglia and thalamus?
A) Arteriovenous malformation (AVM)
B) Charcot-Bouchard aneurysm
C) Cerebral amyloid angiopathy (CAA)
D) Venous sinus thrombosis
E) Subarachnoid haemorrhage
Question 31:
Which of the following is NOT a type of declarative memory?
- Semantic
- Episodic
- Procedural
- Working memory
- Short term memory
Question 32:
Baum’s loop consists of optic radiation fibres that transmit information from the retina to the visual cortex. Which of the following statements about Baum’s loop is correct?
A) Carries information from the superior retinal field, corresponding to the inferior visual field in the visual cortex, and passes through the parietal lobe.
B) Carries information from the superior retinal field, corresponding to the inferior visual field in the visual cortex, and passes through the temporal lobe.
C) Carries information from the inferior retinal field, corresponding to the superior visual field in the visual cortex, and passes through the parietal lobe.
D) Carries information from the inferior retinal field, corresponding to the superior visual field in the visual cortex, and passes through the temporal lobe.
E) Carries information from the superior retinal field, corresponding to the superior visual field in the visual cortex, and passes through the parietal lobe
Question 33:
What is the 2nd stage of otitis media?
- Perforation of the tympanic membrane
- Obstruction of the pharyngotympanic tube
- Suppuration
- Congestion/hyperaemia
- Appearance of bubbles on the tympanic tube
Question 34:
Which of the following arteries supplies the genu of the internal capsule?
- Lateral striate branches of the middle cerebral artery
- Middle striate branches of the anterior cerebral artery & branches of internal carotid artery
- Middle striate branches of the middle cerebral artery & branches of internal carotid artery
- Middle striate branches of the anterior cerebral artery
- Anterior choroidal artery
Question 35:
Which of the following is not a symptom of acute rise in intracranial pressure?
- Papillodeama
- Cushing’s triad
- Headache that come on when coughing/sneezing (Valsalva)
- Gait abnormalities
- Pulsatile tinnitus
Question 36:
Which of the following diseases is characterised by bilateral loss of pain & temperature sensations in a ‘cape like’ distribution?
- Syringomyelia
- Sensory polyneuropathy
- Sensory neuronopathy
- Radiculopathy
- Brown Sequard Syndrome
Question 37:
Which of the following structures connects Broca’s area to Wernicke’s area?
- Medial longitudinal fasciculus
- Medial lemniscus
- Arcuate fasciculus
- Meyer’s fibres
- There are no physical fibres that connect Broca’s & Wernicke’s area
Question 38:
Which of the following disorders is characterised by paralysis / severe weakness of the lower limbs? Which level of the spinal cord is affected?
- Quadraplegia above the level of T2
- Hemiplegia below the level of T2
- Paraplegia below the level of T2
- Monoplegia below the level of T2
- Hemiplegia below the level of C6
Question 39:
Damage to which part of the body causes hemiplegia?
- Internal capsule
- Synapse between UMN & LMN
- Pyramids of the medulla oblongata
- Primary motor cortex
- Corona radiata
Question 40:
Which of the following is not a cause of labyrinthitis?
- Measles
- Mumps
- Rubella
- Meningitis
- Complications of otitis media
Question 41:
Which of the following is a voluntary tract responsible for head & neck movement?
- Rubrospinal tract
- Corticospinal tract
- Tectospinal tract
- Reticulospinal tract
- Corticobulbar tract
Question 42:
Which of the following is characterised by degeneration of the cochlear end organs?
- Presbyacusis
- Labyrinthitis
- Vestibular schwannoma
- Aplasia
- Atresia
Question 43:
Which of the following haemorrhages is characterised by a thunderclap headache aka the worst headache of my life?
- Epidural haemorrhage
- Subdural haemorrhage
- Subarachnoid haemorrhage
- Intracerebral haemorrhage
- Charcot Bouchard haemorrhage
Question 44:
Which of the following is a virus that does NOT cause meningitis?
- Herpes simplex virus type 1
- Herpes simplex virus type 2
- HIV
- Enterovirus
- Toxoplasma
Question 45:
Which of the following is not a medical emergency characterised by gradual loss of vision?
- Vitreous haemorrhage
- Retinal vein occlusion
- Macular degeneration
- Retinal detachment
- Closed angle glaucoma
Question 46:
Which of the following is the main vessel affected by a subarachnoid haemorrhage?
- Middle meningeal artery
- Middle cerebral artery
- Middle cerebellar artery
- Maxillary artery
- Anterior cerebral artery
Question 47:
In the basal ganglia, what neurotransmitter does the subthalamic nucleus usually release?
- GABA
- Glutamate
- Dopamine
- Acetylcholine
- Substance P
Question 48:
What is the name of the dural fold that separates the cerebellum from the cerebrum?
- Falx cerebri
- Falx cerebelli
- Tentorium cerebelli
- Calcarine sulcus
- Diaphragm sellae
Question 49:
Which of the following is spared in spinal artery syndrome?
- Pain
- Temperature
- Crude touch
- Fine touch
- Motor function
Question 50:
Which of the following neurotransmitters is thought to increase pain in the dorsal root ganglia of C fibres?
- Glutamate
- Substance P
- Cholecystokinin
- Galanin
- Nitric oxide
Question 51:
Which of the following is the main factor that causes complete CN III palsy (damage to the central fibres of the oculomotor nerve)?
- Microvascular disease
- Compression e.g., by tumours
- Meningitis
- Neurodegenerative disease
- Haemorrhage
Question 52:
Which of the following areas of the midbrain is the primary control centre of descending pain?
- Medial lemniscus
- Periaqueductal grey matter
- Superior colliculus
- Cerebral peduncles
- Medial longitudinal fasciculus
Question 53:
Which extraocular muscle is particularly vital in the convergence phase of the accommodation reflex? (Hint: think about the position of the eyes in refractive convergent strabismus in children).
- Ciliary muscle
- Levator palpebrae superioris
- Medial rectus
- Lateral rectus
- Superior rectus
Question 54:
Which eye condition is the image showing?
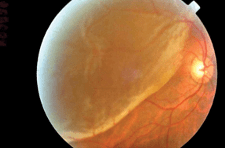
- Retinal detachment
- Diabetic retinopathy
- Retinal vein occlusion
- Retinal artery occlusion
- Glaucoma
Question 55:
A 12-year-old boy presents with progressive ataxia, dysarthria, and lower limb weakness. His condition is associated with cardiomyopathy and diabetes mellitus. Genetic testing reveals a mutation in the FXN gene. What is the most likely diagnosis?
A) Duchenne Muscular Dystrophy
B) Friedreich’s Ataxia
C) Parkinson’s disease
D) Huntington’s Disease
E) CMT-X1
Question 56:
A 50-year-old man presents with headaches, nausea, and seizures. MRI reveals a solitary enhancing lesion in the left frontal lobe with surrounding edema. A biopsy confirms a diagnosis of glioblastoma multiforme. Which of the following statements best describes the nature of this tumour and its potential complications?
A) It arises from oligodendrocytes and is typically slow-growing with minimal metastasis outside the brain
B) It arises from astrocytes and is highly aggressive, often crossing the corpus callosum
C) It primarily originates from peripheral nervous system Schwann cells and is commonly associated with neurofibromatosis type 2
D) It is a secondary tumour, commonly metastasising from a lung carcinoma
E) It arises from meningeal cells and is commonly benign, compressing adjacent brain structures
Question 57:
Which of the following statements regarding Lambert-Eaton Myasthenic Syndrome (LEMS)?
A) LEMS is primarily caused by direct damage to the neuromuscular junction.
B) LEMS is often associated with small cell lung carcinoma (SCLC).
C) Symptoms of LEMS include only muscle weakness without any autonomic dysfunction.
D) LEMS can be treated effectively with antibiotics.
E) LEMS is an autoimmune disorder that primarily affects the peripheral nervous system.
Question 58:
Which of the following statements about refractive errors of the eye is TRUE?
A) Myopia (near-sightedness) is caused by an excessively short eyeball.
B) Hyperopia (farsightedness) typically leads to difficulty seeing objects up close.
C) Astigmatism is primarily caused by a perfectly spherical cornea.
D) Presbyopia is a refractive error that can be corrected with laser surgery.
E) All refractive errors can be effectively corrected using the same type of lenses.
Question 59:
A 55-year-old man presents with progressive weakness and muscle atrophy in his hands and arms, as well as muscle fasciculations. He has also noticed increasing difficulty with swallowing and slurred speech. There is no family history of similar symptoms.
Neurological examination reveals hyperreflexia in addition to muscle atrophy and fasciculations. Which of the following is the most likely diagnosis?
A)Spinal Muscular Atrophy (SMA)
B) Primary Lateral Sclerosis (PLS)
C) Amyotrophic Lateral Sclerosis (ALS)
D) Multiple Sclerosis (MS)
E) Myasthenia Gravis (MG)
Question 60:
A 48-year-old woman is found to have a left superior quadrantanopia on visual field testing. Which of the following is the most likely location of the lesion?
A) Right Parietal Lobe
B) Right Temporal Lobe
C) Left Occipital Lobe
D) Optic Chiasm
E) Right Optic Nerve
Question 61:
A 2-year-old child is brought to the paediatrician by their parents, who have noticed a white reflection in the child’s left pupil in photographs. The child has also been bumping into objects on the left side. Which of the following is the most likely cause of leukocoria in this case?
A) Congenital Cataract
B) Retinoblastoma
C) optic neuritis
D) Glaucoma
E) Retinal Detachment
Question 62:
A 45-year-old woman presents with a six-month history of hearing loss in her right ear, along with a sensation of fullness and occasional ringing. She denies drainage from the ear. On examination, her tympanic membrane appears intact but retracted. There is no fever or evidence of infection. Audiometry reveals conductive hearing loss on the right side. Which of the following is the most likely diagnosis?
A) Otosclerosis
B) Acute Otitis Media
C) Cholesteatoma
D) Meniere’s Disease
E) Eustachian Tube Dysfunction
Question 63:
A 67-year-old man presents to the emergency department with a sudden onset of right-sided numbness and tingling involving his face, arm, and leg. He also reports difficulty with concentration and mild confusion. His speech is intact. Brain imaging reveals a small infarction in the left thalamus. Which of the following is the most likely symptom this patient will experience due to his thalamic infarction?
A) ipsilateral (left) Hemiparesis
B) Hemianopia
C) right sided Hemisensory Loss
D) Aphasia
E) Ataxia
Question 64:
A 35-year-old man presents with severe, excruciating pain around his right eye that started suddenly 30 minutes ago. He reports that these headaches occur daily for the past week, lasting around 45 minutes each, and often wake him up at night. He has associated tearing, rhinorrhea, and eye redness on the same side. Which of the following is the most likely diagnosis?
A) Migraine
B) Tension Headache
C) Cluster Headache
D) Temporal Arteritis
E) Trigeminal Neuralgia
Question 65:
A 24-year-old man presents to the emergency department with a severe headache, high fever, photophobia, and neck stiffness. His family reports that he has become increasingly confused over the past few hours. A lumbar puncture is performed, and cerebrospinal fluid (CSF) analysis shows elevated protein, decreased glucose, and a high white blood cell count with predominantly neutrophils. What is the most likely diagnosis?
A) Bacterial encephalitis
B) Bacterial Meningitis
C) Brain Abscess
D) Viral Encephalitis
E) Fungal Meningitis
Question 66:
A 57-year-old right-handed woman is brought to the emergency department by her family due to difficulty speaking. She understands spoken language and can follow commands but struggles to repeat sentences accurately. She appears frustrated, as her speech contains frequent pauses and incorrect word substitutions. She has no muscle weakness, and her comprehension and motor skills are intact. What is the most likely diagnosis?
A) Broca’s aphasia
B) Wernicke’s aphasia
C) Guillain Barre syndrome
D) Conduction aphasia
E) Friedreich’s ataxia
Question 67:
A 34-year-old man is brought to the emergency department after being involved in a motorcycle accident. On examination, he has weakness in his right leg and a loss of vibration and proprioception on the same side (right side). He also has loss of pain and temperature sensation on the left side of his body below the T10 level. What is the most likely diagnosis?
A) Amyotrophic lateral sclerosis (ALS)
B) Guillain-Barré syndrome
C) Multiple sclerosis
D) Brown-Séquard syndrome
E) Anterior spinal artery syndrome
Question 68:
A 22-year-old male presents to the emergency department after a high-speed car accident. He briefly lost consciousness at the scene. A few hours later, he developed a severe headache, nausea, and progressive drowsiness. He experienced drunk-like symptoms. On examination, he has a dilated pupil on the right side and weakness in his left arm and leg. A CT scan of the head shows a biconvex (lentiform) hyperdensity. What is the most likely diagnosis?
A) Subarachnoid haemorrhage
B) Epidural haemorrhage
C) Subdural haemorrhage
D) Cerebral contusion
E) Intracerebral haemorrhage
Question 69:
A 65-year-old man presents with increasing difficulty in initiating movement, tremors in his hands, and stiffness in his muscles. His family notes that his facial expressions have become less animated, and his handwriting has become smaller. On examination, he has a resting tremor in both hands, bradykinesia (slowness of movement), and increased resistance to passive movement in his limbs. What is the most likely diagnosis?
A) Amyotrophic lateral sclerosis (ALS)
B) Huntington’s disease
C) Multiple system atrophy (MSA)
D) Parkinson’s disease
E) Wilson’s disease
Question 70:
A 72-year-old man is brought to the clinic by his wife due to progressive memory problems over the past year. He experiences frequent episodes of confusion, vivid visual hallucinations, and fluctuating levels of alertness throughout the day. His wife has also noticed that he has developed stiffness in his limbs and a shuffling gait. On examination, he has mild bradykinesia and features of Parkinsonism. What is the most likely diagnosis?
A) Alzheimer’s disease
B) Vascular dementia
C) Lewy body dementia
D) Frontotemporal dementia
E) Normal pressure hydrocephalus
Question 71:
A 25-year-old man presents with slowly progressive weakness and wasting in his lower legs, causing difficulty walking. He mentions that his foot arches have become increasingly high and he frequently trips due to “foot drop.” His father had similar issues starting in his twenties. On examination, there is distal muscle wasting, diminished deep tendon reflexes, and decreased sensation in a stocking-glove distribution. Nerve conduction studies reveal slowed conduction velocities. What is the most likely diagnosis?
A) Charcot-Marie-Tooth disease type 1 (CMT1)
B) Spinal Muscular Atrophy
C) Guillain-Barré syndrome (GBS)
D) Amyotrophic Lateral sclerosis
E) Hereditary spastic paraplegia (HSP)
Question 72:
A 68-year-old woman is brought to the clinic by her daughter due to difficulty performing simple tasks like brushing her hair, despite understanding what she is supposed to do. She can describe how to perform the action, but when asked to demonstrate, she struggles to execute the correct movements. Neurological examination reveals no weakness or sensory loss. What is the most likely type of apraxia?
A) Ideomotor apraxia
B) Ideational apraxia
C) Constructional apraxia
D) Buccofacial apraxia
E) Limb-kinetic apraxia
Question 73:
A 30-year-old woman presents with progressive headaches, neck pain, and difficulty with balance and coordination over the past few months. She also reports dizziness, and occasional blurry vision. Neurological examination reveals impaired coordination and mild weakness in the lower extremities. MRI of the brain reveals herniation of the cerebellum through the foramen magnum. What is the most likely cause of her hydrocephalus?
A) Arnold-Chiari malformation
B) Meningitis
C) Choroid plexus papilloma
D) Subarachnoid haemorrhage
E) Aqueductal stenosis
Question 74:
A 35-year-old man is brought to the emergency department with a sudden-onset headache, weakness on the right side of his body, and confusion. A CT scan of the head reveals an intracerebral haemorrhage in the right hemisphere. Which of the following is the most likely underlying cause of his intracerebral haemorrhage?
A) Hypertension
B) Cerebral amyloid angiopathy
C) Arteriovenous malformation
D) Coagulopathy
E) Trauma
Question 75:
Which of the following mechanisms is most associated with the pathophysiology of Huntington’s disease?
a) Loss of function mutations in mitochondrial DNA
b) Trinucleotide expansion of CAG repeats leading to toxic gain of function
c) Antibody-mediated destruction of voltage-gated calcium channels
d) Autosomal recessive inheritance leading to enzyme deficiencies
e) Mutation in nuclear frataxin gene impairing mitochondrial function
Question 75:
A patient presents with progressive muscle weakness and is diagnosed with Myasthenia Gravis. The pathophysiology of this condition primarily involves:
a) Autoantibodies against presynaptic calcium channels
b) Autoantibodies against postsynaptic acetylcholine receptors
c) Trinucleotide repeat expansion leading to glutamine accumulation
d) Mitochondrial dysfunction leading to impaired ATP production
e) Antibody-mediated damage to the blood-brain barrier
Question 76:
Which of the following best describes the pathophysiology of paraneoplastic syndromes?
a) Direct metastasis of cancer cells to the CNS
b) Inflammatory damage due to tumour necrosis
c) Autoimmune attack on nervous system structures triggered by tumour antigens
d) Increased intracranial pressure due to space-occupying lesions
e) Compression of the spinal cord by a tumour
Question 77:
Which of the following neurotransmitters is primarily inhibitory in the central nervous system?
a) Acetylcholine
b) Glutamate
c) GABA
d) Dopamine
e) Serotonin
Question 78:
A patient with a mitochondrial disorder most likely exhibits which of the following symptoms?
a) Chronic liver failure
b) Muscle weakness and exercise intolerance
c) Hypertension
d) Haemolytic anaemia
e) Peripheral neuropathy without motor involvement
Question 79:
In Parkinson’s disease, which of the following is the primary neurotransmitter deficiency?
a) Serotonin
b) Acetylcholine
c) Dopamine
d) Glutamate
e) GABA
Question 80:
Which of the following types of neoplastic progression is most closely associated with the loss of cellular differentiation and aggressive growth?
a) Hyperplasia
b) Metaplasia
c) Dysplasia
d) Anaplasia
e) Hypertrophy
Question 81:
In Huntington’s Disease, the pathological accumulation of abnormal huntingtin protein is most likely to affect which brain region?
a) Cerebellum
b) Substantia nigra
c) Hippocampus
d) Basal ganglia
e) Motor cortex
Question 82:
A patient presents with signs of a haemorrhagic stroke. What is the most common cause of subarachnoid haemorrhage in young adults?
a) Rupture of an arteriovenous malformation
b) Intracerebral haemorrhage due to hypertension
c) Ruptured berry aneurysm
d) Subdural hematoma from trauma
e) Cortical vein thrombosis
Question 83:
Which of the following is a key risk factor for lacunar infarcts in small vessel ischemic stroke?
a) Atrial fibrillation
b) Diabetes mellitus
c) Hyperlipidemia
d) Hypertension
e) Obesity
Question 84:
Which of the following is a classic sign of raised intracranial pressure (ICP)?
a) Decorticate posturing
b) Cushing’s triad
c) Positive Romberg’s sign
d) Diplopia
e) Bradykinesia
Question 85:
Which of the following conditions is most likely to present with a sudden onset “thunderclap” headache?
a) Lacunar infarct
b) Subarachnoid hemorrhage
c) Brain abscess
d) Ischemic stroke
e) Tension headache
Question 86:
Communicating hydrocephalus is typically associated with which of the following symptoms?
a) Hemiplegia, aphasia, and sensory loss
b) Headache, papilledema, and vomiting
c) Gait disturbance, cognitive decline, and urinary incontinence
d) Neck stiffness, fever, and photophobia
e) Seizures, confusion, and hemiparesis
Question 87:
A 70-year-old patient presents with sudden onset of right-sided weakness and slurred speech. CT scan confirms a stroke. Which artery is most likely involved based on the symptoms?
a) Anterior cerebral artery
b) Middle cerebral artery
c) Posterior cerebral artery
d) Basilar artery
e) Lenticulostriate arteries
Question 88:
Which neurological sign is indicative of meningeal irritation in a patient suspected of having meningitis?
a) Babinski’s sign
b) Kernig’s sign
c) Homan’s sign
d) Romberg’s sign
e) Lhermitte’s sign
Question 89:
A 25-year-old male presents with sudden-onset headaches described as “thunderclap” and a stiff neck. What is the most appropriate initial imaging study to rule out subarachnoid haemorrhage?
a) MRI of the brain
b) CT scan of the brain
c) X-ray of the cervical spine
d) Ultrasound of the carotids
e) Lumbar puncture
Question 90:
Which type of hydrocephalus is characterized by an accumulation of cerebrospinal fluid (CSF) due to impaired absorption rather than obstruction?
a) Non-communicating hydrocephalus
b) Communicating hydrocephalus
c) Normal pressure hydrocephalus
d) Acute hydrocephalus
e) Congenital hydrocephalus
Question 91:
Which of the following diseases is most characteristically associated with bradykinesia and rigidity?
a) Huntington’s disease
b) Amyotrophic lateral sclerosis
c) Progressive supranuclear palsy
d) Parkinsonism
e) Corticobasal degeneration
