
Urogenital
Question 1:
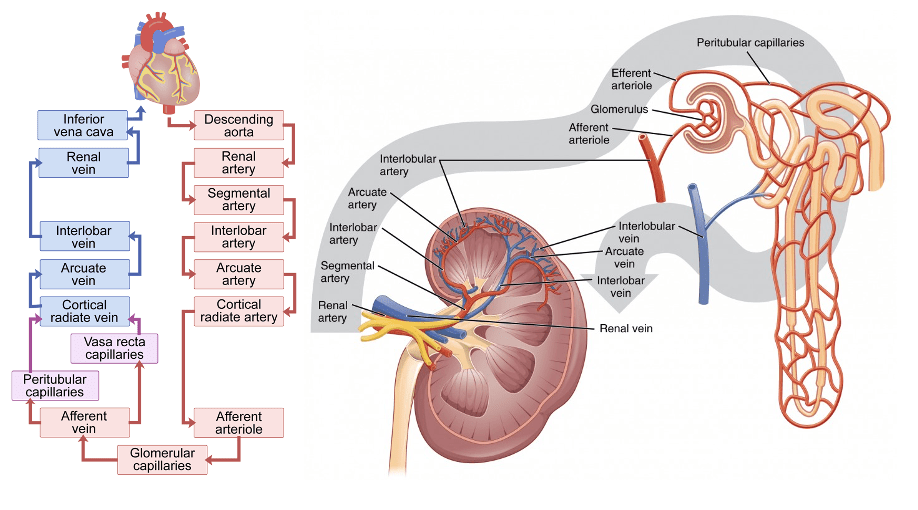
**Answer: E) Interlobular artery/ Cortical radiate artery**
*Explanation: The interlobular (cortical radiate) arteries are the ones that extend into the renal cortex and distribute blood to the afferent arterioles of the nephrons from the interlobar arteries.
A is incorrect as the interlobar artery arises from the segmental artery and travels through the renal columns between the renal pyramids. It does not directly supply the renal cortex but rather give rise to the arcuate arteries.
B is incorrect as the arcuate artery forms arcs along the boundary between the renal cortex and the renal medulla. It does not directly carry blood into the renal cortex; instead, it gives rise to the interlobular artery (Cortical radiate artery).
C is incorrect as the segmental artery is the first branch of the renal artery, it does not carry blood to the renal cortex though.
D is incorrect as the efferent arteriole carries blood away from the glomerulus after filtration has occurred and supplies it to either the peritubular capillaries in the cortex or the vasa recta in the medulla. It does not carry blood into the renal cortex from the renal artery. Mnemonic for arteries and veins of the kidneys.
“Rats Sneak In And Invade Cots” –
R: Renal artery
S: Segmental artery
I: Interlobar artery
A: Arcuate artery
I: Interlobular artery (Cortical radiate artery)
A: Afferent arteriole
“Elephants Invented Awesome Ice Cream Recipes” –
E: Efferent arteriole
I: Interlobular veins (Cortical radiate veins)
A: Arcuate veins
I: Interlobar veins
R: Renal vein
Question 2:
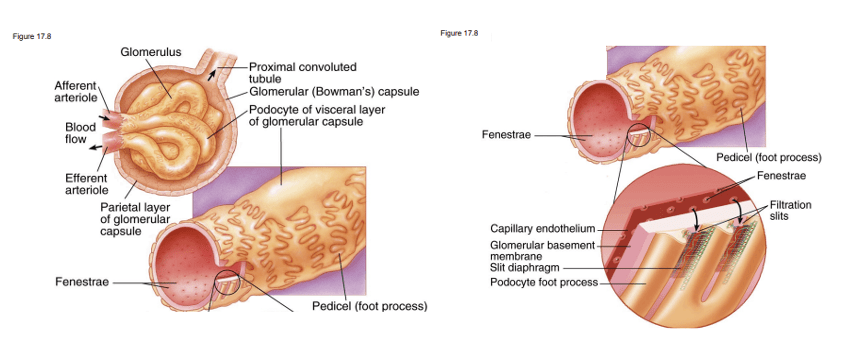
**Answer: A) Podocytes**
*Explanation: Podocytes are specialized cells in the glomerulus that form the visceral layer of Bowman’s capsule and are responsible for the filtration of blood in the renal corpuscle.*
B is incorrect as principal cells are found in the renal tubules and collecting ducts of the nephron. They are involved in the reabsorption and secretion of ions and water, particularly under the influence of hormones like aldosterone and antidiuretic hormone (ADH).
C is incorrect as mesangial cells have contractile properties and can contract or relax to regulate the blood flow through the glomerulus. Contraction of mesangial cells reduces the surface area available for filtration by narrowing the capillary lumens, while relaxation increases filtration surface area by widening the capillary lumens. This contractile activity helps to regulate glomerular filtration rate (GFR) and maintain optimal filtration efficiency. They are also involved in phagocytosis within the glomerulus.
D is incorrect as macula densa cells are specialized cells located in the distal convoluted tubule near the glomerulus. They monitor the concentration of sodium chloride (NaCl) in the filtrate and play a role in regulating the glomerular filtration rate (GFR) and renin secretion in response to changes in NaCl levels, if NaCl concentrations are too low, this indicates low GFR which is detected by the macula densa cells which stimulate the release of renin from juxtaglomerular (granular) cells to increase GFR. E is incorrect as juxtaglomerular (granular) cells are located near the afferent arteriole of the glomerulus. They secrete renin in response to signals such as low blood pressure or low sodium levels, which initiates the renin-angiotensin-aldosterone system (RAAS) to regulate blood pressure, increase GFR and fluid balance.
Question 3:
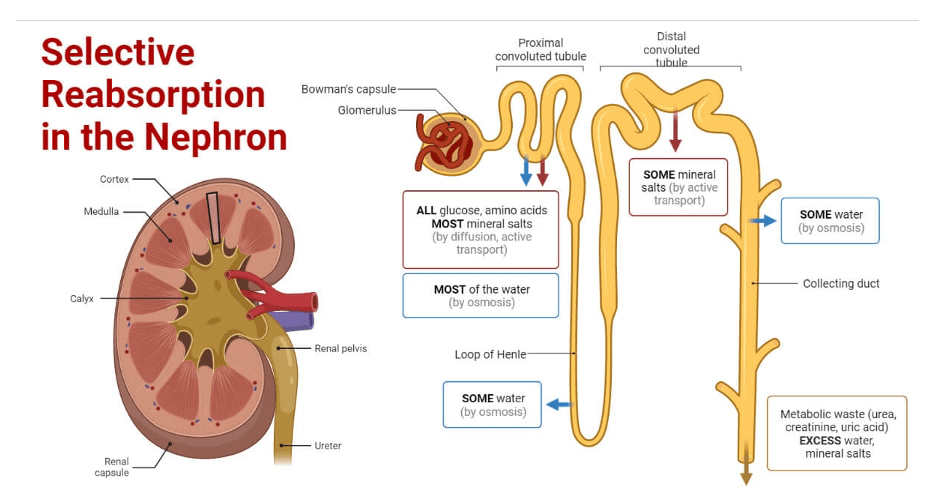
**Answer: C) Proximal convoluted tubule**
*Explanation: The majority of tubular reabsorption occurs in the proximal convoluted tubule, where various solutes and water are reabsorbed into the bloodstream.*
Question 4:
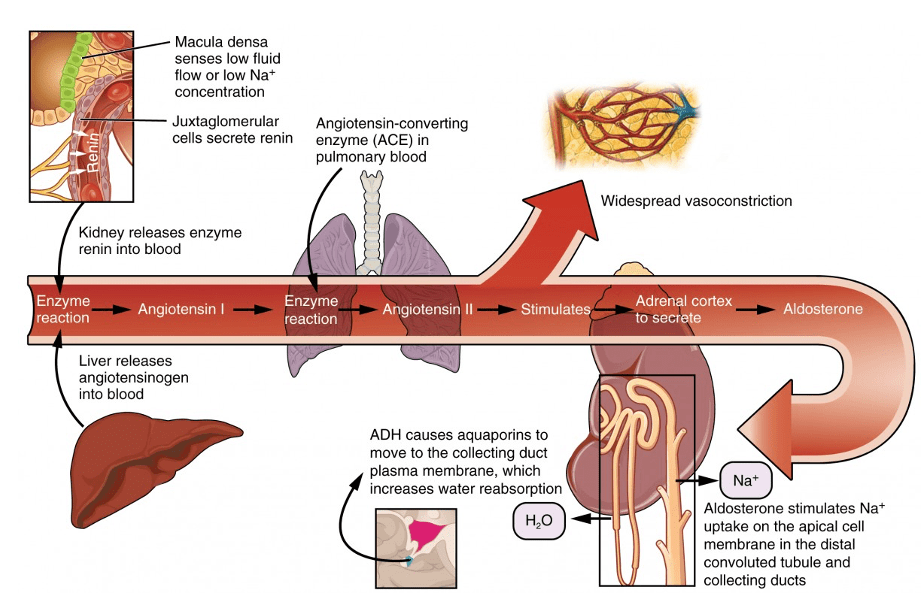
Answer: A) Regulation of blood pressure**
*Explanation: The juxtaglomerular apparatus plays a crucial role in regulating blood pressure by secreting renin in response to changes in blood pressure or sodium levels, detected by Macula densa cells. When levels of sodium chloride in the distal convoluted tubule are low, it indicates that the GFR is low which can be due to low blood pressure, hence the Juxtaglomerular apparatus/cells release renin which promotes systemic vasoconstriction to increase blood pressure, the release of angiotensin from the adrenal glands, as this stimulates more sodium reabsorption from DCT and collecting ducts causing water to move in by osmosis which increases blood volume and hence blood pressure, it also stimulates the release of ADH (vasopressin) from the posterior pituitary which stimulates the formation of aquaporins in the collecting ducts, causing more water to be absorbed, increasing the volume of blood and therefore blood pressure.*
Question 5:
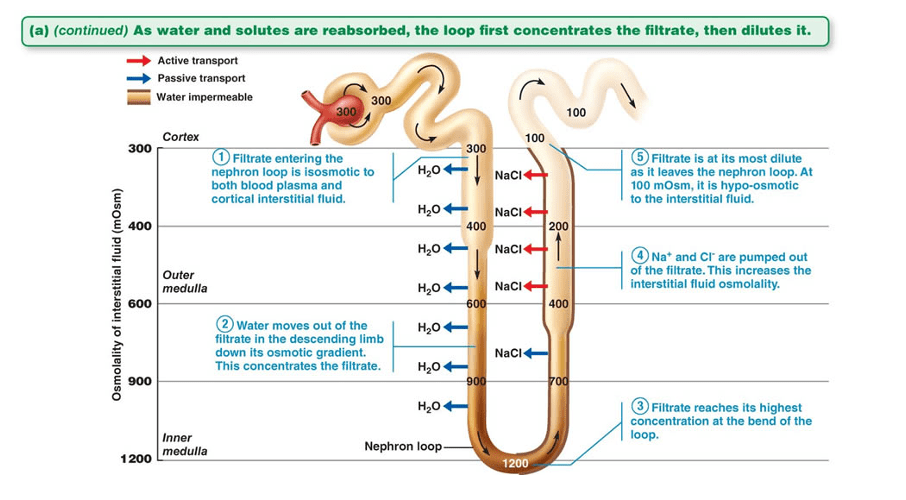
Answer: C) Ascending limb of the loop of Henle**
*Explanation: The ascending limb of the loop of Henle is impermeable to water and actively reabsorbs ions like sodium and chloride.*
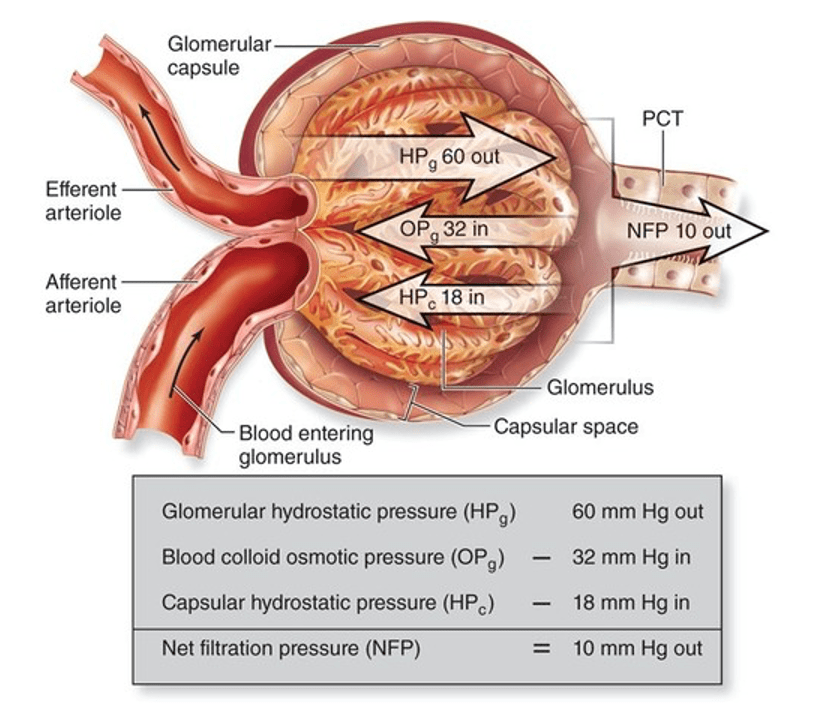
Question 6:
Answer: C) 32 mmHg.
Explanation: Blood colloid osmotic pressure (BCOP), also known as oncotic pressure, is the osmotic pressure exerted by the proteins (especially albumin) present in blood plasma. It is an essential force responsible for maintaining fluid balance between the blood vessels and tissues. Typically, in a healthy individual, the blood colloid osmotic pressure is around 32 mmHg. This pressure helps to prevent excessive loss of fluid from the bloodstream into the surrounding tissues, thereby contributing to the regulation of blood volume and blood pressure. Any significant deviation from this value can lead to fluid imbalances and various health complications.
A is incorrect as this is the net filtration pressure.
B is incorrect as this is the capsular hydrostatic pressure.
D is incorrect as this is the glomerular hydrostatic pressure
Question 7:
The correct answer is C) Hypoxia.
Explanation: Erythropoietin (EPO) is a hormone produced primarily by the kidneys in response to low oxygen levels in the blood (hypoxia). When tissues in the body do not receive enough oxygen, such as in conditions like high altitude or lung disease, the kidneys detect this hypoxic state and release EPO into the bloodstream. EPO then stimulates the bone marrow to produce more red blood cells, which helps to increase the oxygen-carrying capacity of the blood. This feedback loop ensures that oxygen delivery to tissues is maintained within a normal range. Therefore, hypoxia is the main driver to produce erythropoietin.
A is incorrect as hyperglycaemia is high blood glucose levels. It primarily stimulates insulin release from the pancreas, aiming to lower blood glucose levels by facilitating glucose uptake into cells.
B is incorrect as hypoglycaemia is low blood glucose levels. It stimulates hormones such as glucagon and epinephrine, which work to raise blood glucose levels by promoting glycogen breakdown and glucose release from the liver.
D is incorrect as hypercapnia is high levels of carbon dioxide (CO2) in the blood. It stimulates an increase in respiratory rate and depth, which helps to eliminate excess CO2 from the body and restore normal blood pH.
E is incorrect as acidosis is a condition where there is an excessive accumulation of acid in the body or a decrease in blood pH. It stimulates respiratory compensation (increased ventilation) and renal compensation (increased excretion of hydrogen ions and reabsorption of bicarbonate ions) to restore acid-base balance.
Question 8:
**Answer: B) Arcuate artery**
*Explanation: The arcuate artery supplies oxygenated blood directly to the medullary region of the kidney, located at the boundary between the cortex and medulla.*
Question 9:
**Answer: B) Distal convoluted tubule**
*Explanation: The distal convoluted tubule is responsible for the secretion of hydrogen ions and the reabsorption of bicarbonate ions in urine, helping to regulate acid-base balance.*
A is partially incorrect as the proximal convoluted tubule is primarily responsible for reabsorption of ions, glucose, amino acids, and water from the filtrate back into the bloodstream. It also secretes substances into the filtrate, but it does not specifically handle hydrogen ions and bicarbonate ions to the extent that the distal convoluted tubule does. Therefore, this is not the best answer.
C is incorrect as the loop of Henle is involved in reabsorption of water and electrolytes (sodium, chloride) from the filtrate, but it does not play a direct role in the secretion of hydrogen ions or reabsorption of bicarbonate ions.
D is incorrect the collecting duct is responsible for further reabsorption of water and electrolytes under the influence of hormones like antidiuretic hormone (ADH) and aldosterone. It does not directly secrete hydrogen ions or reabsorb bicarbonate ions.
E is incorrect as the glomerulus is a network of capillaries where filtration of blood occurs to form the initial filtrate that enters the nephron, but it does not have a role in the secretion of hydrogen ions or reabsorption of bicarbonate ions.
Question 10:
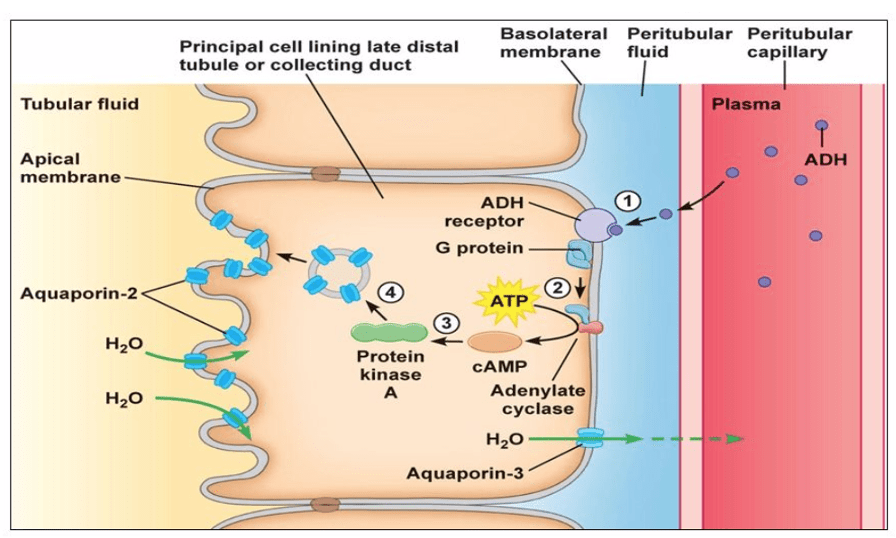
The correct answer is D) By upregulating the expression of aquaporin channels.
Explanation: Vasopressin, also known as antidiuretic hormone (ADH), plays a crucial role in regulating water balance in the body. It is released in response to signals such as increased blood osmolality (concentration) or decreased blood volume. One of its primary actions is to increase water reabsorption in the kidneys, primarily in the collecting ducts. Vasopressin achieves this by upregulating the expression of aquaporin channels (Aquaporin 2 on the apical side and Aquaporin 3 on the basolateral side) in the cells lining the collecting ducts. Aquaporins are water channels that facilitate the movement of water across cell membranes. By increasing the number of aquaporin channels, vasopressin enhances the permeability of the collecting ducts to water, allowing for more efficient reabsorption of water from the urine back into the bloodstream. This mechanism helps to conserve water and concentrate urine, thereby maintaining proper fluid balance in the body.
A is incorrect as this describes the function of aldosterone not vasopressin.
B is incorrect as vasopressin has no function related to potassium excretion.
C is incorrect as this describes the function of angiotensin II not vasopressin.
E is incorrect as Vasopressin is the same as ADH, so it won’t inhibit its own secretion.
Question 11:
**Answer: E) Water**
*Explanation: The descending limb of the loop of Henle is permeable to water and allows for the passive reabsorption of water, concentrating the filtrate.
** Question 12:**
The correct answer is C) Elevation of the scrotum and testes towards the body.
Explanation: The cremaster muscle is a thin layer of skeletal muscle found within the spermatic cord and surrounding the testes. Its primary function is to elevate the scrotum and testes towards the body. This action helps to regulate the temperature of the testes by bringing them closer to the body when it’s cold and lowering them away from the body when it’s warm. This temperature regulation is crucial for maintaining optimal sperm production and function.
Question 13:
**Answer: C) Reabsorption of water**
*Explanation: Collecting ducts play a crucial role in reabsorbing water from the urine, allowing the body to regulate its fluid balance and concentrate urine.*
A is incorrect as this is the function of the glomerulus.
B is incorrect as reabsorption of glucose mainly occurs in the proximal convoluted tubule not in the collecting ducts.
D is incorrect as renin secretion is stimulated by juxtaglomerular cells located on the afferent arteriole not in the collecting ducts.
E is incorrect as regulation of blood pressure is influenced primarily by renin secretion from juxtaglomerular cells in the afferent arteriole and the detection of low blood pressure occurs by macula densa cells on the distal convoluted tubule.
** Question 14:**
**Answer: A) Simple squamous epithelium**
*Explanation: The renal corpuscle consists of a simple squamous epithelium in the form of the parietal layer of Bowman’s capsule and endothelial cells lining the glomerular capillaries. These cells are fenestrated (have pores) to allow for filtration of very small molecules (under 3000 Daltons) from the blood plasma.*
** Question 15:**
*Answer: C) Prolactin**
*Explanation: Prolactin is the primary hormone responsible for initiating and maintaining lactation, including milk production in the mammary glands during pregnancy and post-partum.*
A is incorrect as oestrogen plays a role in breast development during pregnancy but is not primarily responsible for milk production.
Progesterone helps prepare the breast tissue for lactation during pregnancy but does not stimulate milk production
D is incorrect as oxytocin is involved in the let-down reflex, which is the release of milk from the mammary glands to the nipple during breastfeeding. It stimulates the contraction of myoepithelial cells around the mammary glands, allowing milk to be ejected, but prolactin is what stimulates production of the milk in the first place.
Lactase is an enzyme produced in the intestines that helps digest lactose, the sugar found in milk. It is not a hormone and is not involved in milk production in the mammary glands.
Question 16:
**Answer: C) Muscularis**
*Explanation: The muscularis (muscle) layer of the urinary bladder wall contains the detrusor muscle, which contracts during micturition to expel urine.*
Question 17:
**Answer: B) Relaxing to allow urine to flow into the urethra **
*Explanation: The internal urethral sphincter relaxes to allow urine to enter the urethra. Under normal conditions, the internal urethral sphincter remains tonically contracted to maintain urinary continence and prevent involuntary urination (via the hypogastric nerve innervation). During the micturition reflex (urination process), when the bladder contracts (due to activation of the detrusor muscle) and the pressure within the bladder increases, stretch receptors in the bladder wall signal the nervous system. This signal leads to relaxation of the internal urethral sphincter, allowing urine to flow from the bladder into the urethra (due to pelvic splanchnic nerve). The external urethral sphincter, which is under voluntary control (somatic nervous system), remains voluntarily contracted (innervated by the pudendal nerve) until we are in the correct setting. *
A is incorrect as the micturition reflex is initiated by distention receptors
C is incorrect as this describes the function of the internal urethral sphincter when not in micturition, under normal conditions.
D is incorrect as this occurs by stretch receptors in the bladder.
E is incorrect as parasympathetic nervous system (pelvic splanchnic nerve roots S2-S4) signals are involved in stimulating bladder contraction (detrusor muscle) during micturition and are initiated by the stretch receptors.
** Question 18:**
The correct answer is C) 50%.
Explanation: Creatinine is a waste product generated from the breakdown of creatine phosphate in muscles. It is filtered out of the blood by the kidneys and excreted into the urine. Elevated levels of creatinine in the blood can be indicative of impaired kidney function. An increase in creatinine levels by 50% from baseline is considered significant and suggestive of kidney damage. This percentage increase reflects a decrease in the kidneys’ ability to filter and excrete creatinine, indicating a decline in renal function.
Question 19:
**Answer: B) Paramesonephric duct (Mullerian duct)**
*Explanation: The paramesonephric duct, also known as the Mullerian duct, gives rise to the female reproductive tract, including the ovaries, uterus, cervix, and upper vagina.*
A is incorrect as in males, the Wolffian ducts develop into the epididymis, vas deferens, and seminal vesicles under the influence of testosterone, but in females it regresses due to the absence of the SRY gene. In embryonic development it does contribute to kidney development in both males and females but once the metanephros forms, the mesonephros regresses in females due to the lack of Y chromosome and SRY gene located on it.
C is incorrect as the urethral folds contribute to the formation of the labia minora in females and corpus spongiosum in males.
D is incorrect as the labioscrotal swellings develops into the labia majora in females and the scrotum in males, but it does not give rise to the internal reproductive organs.
E is incorrect as the phallus develops into the penis in males and the clitoris in females, but it does not give rise to the internal reproductive organs.
Question 20:
**Answer: D) Passage for sperm into the uterus**
*Explanation: The cervix serves as a passage for sperm to enter the uterus and also acts as a barrier to prevent pathogens from entering the reproductive tract.*
A is incorrect oestrogen is primarily produced by the granulosa cells in the ovaries. These cells convert androgens (produced by the theca interna cells) into oestrogen through a process called aromatization. The cervix itself does not produce much oestrogen. Instead, oestrogen influences the cervical mucus production and the structural changes in the cervix during the menstrual cycle.
B is incorrect as ovulation is the release of a mature egg (oocyte) from the ovary, from a follicle that has developed under the influence of follicle-stimulating hormone (FSH) and released due to luteinizing hormone (LH) from the pituitary gland. This process occurs within the ovary and is not directly controlled by or involving the cervix.
C is partially incorrect as fertilization typically occurs in the fallopian tubes (oviducts), where sperm meet the egg after ovulation. While the cervix provides a pathway for sperm to travel from the vagina into the uterus and toward the fallopian tubes, fertilization itself does not occur in the cervix.
E is incorrect as progesterone is primarily produced by the corpus luteum in the ovaries following ovulation. It prepares the uterus for implantation of a fertilized egg and helps maintain pregnancy. The cervix does not produce progesterone.
Question 21:
**Answer: D) Mucosa**
*Explanation: The mucosa layer of the bladder wall is responsible for producing the mucous lining that protects the inner surface of the bladder from the corrosive effects of urine.*
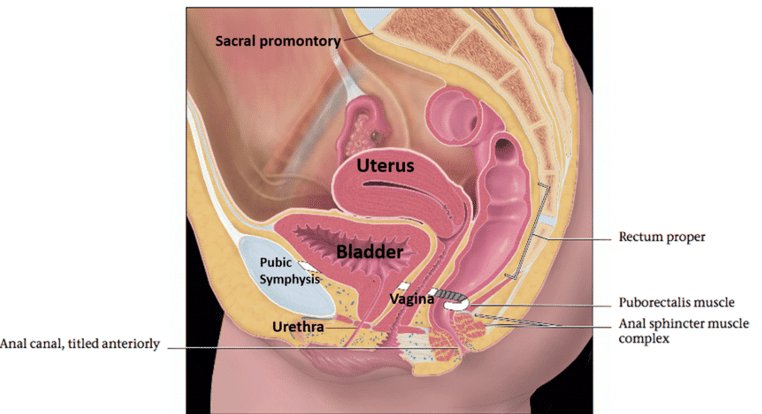
Question 22:
**Answer: B) 3-4 cm, anterior to the vagina**
*Explanation: The female urethra is approximately 3-4 cm in length and is located anterior to the vagina.*
Question 23:
**Answer: C) Spongy (penile) urethra**
*Explanation: The spongy (penile) urethra passes through the corpus spongiosum of the penis and carries both urine and semen.*
Question 24:
**Answer: D) Fallopian tube (oviduct)**
*Explanation: The fallopian tube, also known as the oviduct, is responsible for the fertilization of the egg and the early development of the embryo.*
Question 25:
**Answer: E) Sinus tubercle and Paramesonephric duct **
Explanation: The paramesonephric ducts (Müllerian ducts) fuse with the sinus tubercle to form the uterus, cervix, and upper part of the vagina during embryological development in females. The paramesonephric ducts give rise to the fallopian tubes, uterus, cervix, and upper part of the vagina, while the sinus tubercle contributes to the lower part of the vagina.* Paramesonephric duct=mullerian duct Mesonephric duct=Wolffian Duct.
A is incorrect as the paramesonephric duct (Müllerian duct) does fuse with another structure, but it’s not the Wolffian duct. The Wolffian duct develops into male reproductive structures (epididymis, vas deferens) under the influence of testosterone produced by the testes due to SRY gene in males.
B is incorrect as the urogenital sinus contributes to the formation of the lower part of the vagina and urethra in females but not the upper part of the vagina, uterus, or cervix. The Müllerian duct is not directly involved in the formation of lower vagina and urethra.
C is incorrect as the mesonephric tubules are part of the mesonephros, which is involved in early kidney development and the formation of some male reproductive structures. They do not fuse with the Müllerian duct to form the female reproductive organs.
D is incorrect as the genital tubercle contributes to the formation of the external genitalia in both males and females but does not fuse with the urethral folds to form the internal female reproductive organs.
Question 26:
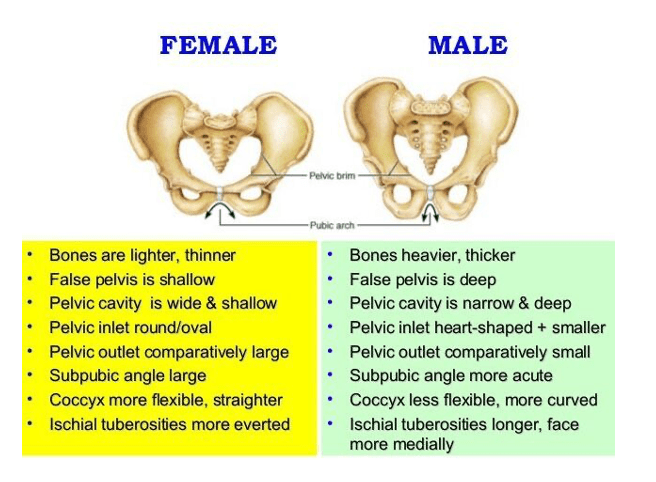
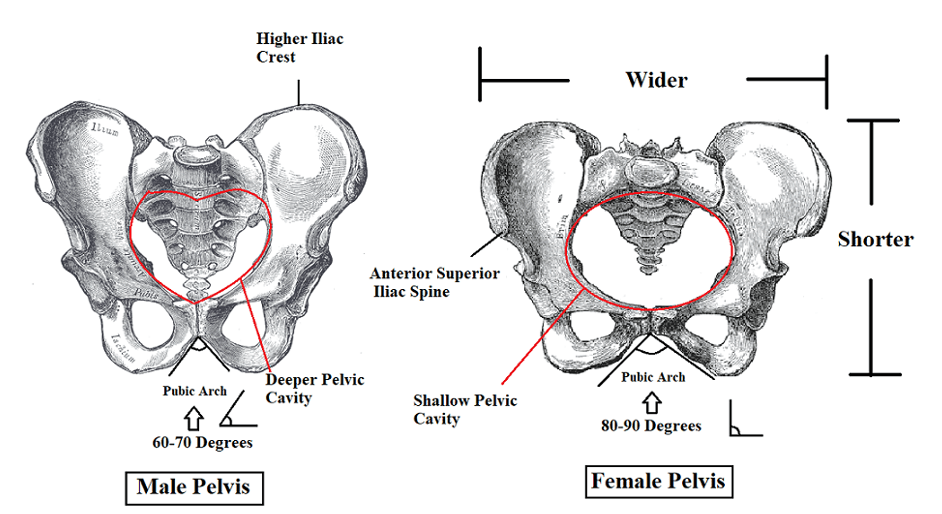
The correct answer is B) The pubic angle is wider in the female pelvis compared to the male pelvis.
Explanation: The pubic angle is the angle formed by the convergence of the two pubic bones at the pubic symphysis. In the female pelvis, the pubic angle is typically wider (greater than 90 degrees) compared to the male pelvis. This wider angle is one of the anatomical adaptations that facilitate childbirth in females by providing more space in the pelvic outlet. Conversely, the male pelvis generally has a narrower pubic angle (less than 90 degrees). This difference in pubic angle is one of the key anatomical distinctions between the male and female pelvises.
Question 27:
**Answer: B) It guides the testis through the inguinal canal.**
*Explanation: The gubernaculum guides the testis from its initial intra-abdominal position through the inguinal canal into the scrotum during embryological descent.*
A is incorrect because the gubernaculum’s role is not to anchor the testis within the abdominal cavity. Instead, it guides the testis during its descent from the abdominal cavity through the inguinal canal into the scrotum. Once the testis reaches the scrotum, the gubernaculum helps anchor it in place within the scrotal sac.
C is incorrect as the gubernaculum does not play a role in promoting the growth of the testis. Testicular growth and development are primarily controlled by hormonal signals such as testosterone.
D is incorrect as testosterone secretion is primarily the function of Leydig cells within the testis. The gubernaculum is a structure made of connective tissue and does not have endocrine functions like hormone secretion.
E is incorrect as sperm production (spermatogenesis) occurs within the seminiferous tubules of the testis and is not influenced by the gubernaculum. The gubernaculum’s role is limited to guiding the testis during descent and aiding in its anchorage in the scrotum.
Question 28:
**Answer: B) Corpus cavernosa**
*Explanation: The corpora cavernosa, two erectile tissues in the penis, fill with blood and become engorged, leading to the initiation of an erection in males.*
A is incorrect as the corpus spongiosum is another erectile tissue in the male reproductive system, but its primary function is to keep the urethra open during ejaculation and to aid in the expulsion of semen.
C is incorrect as the prostate gland is involved in the production of seminal fluid, but it does not directly contribute to the erection process.
D is incorrect as the epididymis is a coiled tube where sperm mature and are stored, but it is not involved in erection.
E is incorrect as the vas deferens transports sperm from the epididymis to the ejaculatory duct during ejaculation but is not responsible for erection.
** Question 29:**
**Answer: B) Females have better sphincter control than males.**
*Explanation: Females typically have better sphincter control in the pelvic floor due to slight differences in structure and arrangements.*
Question 30:
**Answer: E) Alveoli**
*Explanation: Alveoli within the breast are responsible for producing milk during lactation. They are composed of glandular tissue and ducts.*
A is incorrect as lactiferous sinuses are reservoirs or storage areas for milk behind the nipple, where milk collects before breastfeeding. They do not produce milk.
B is incorrect as lactiferous ducts are the main ducts that carry milk from the alveoli (milk-producing glands) to the nipple. They transport milk but do not produce it.
C is incorrect as the areola is the darkened area around the nipple. It contains sebaceous glands (Montgomery glands) that produce an oily substance to lubricate the nipple, but it does not produce milk.
D is incorrect as myoepithelial cells surround the alveoli and lactiferous ducts. They contract during milk ejection (letdown reflex) to push milk into the ducts and towards the nipple. While important in milk expulsion, they do not produce milk themselves
Question 31:
**Answer: B) Located at the 4th intercostal space, lateral to the midaxillary line**
*Explanation: The nipple-areola complex is commonly located at the 4th intercostal space, lateral to the midaxillary line, which is the correct surface anatomy of the breast.*
Question 32:
**Answer: B) Three**
*Explanation: The process of labour and childbirth is typically divided into three stages, each with its specific events and physiological changes. First Stage= Labour in early labour contractions begin, cervix starts to dilate and efface, in active labour the contractions intensify, cervix continues to dilate (4-10 cm), the transition phase is the final stage of dilation (10 cm), intense contractions. Second Stage= Delivery, the baby moves down the birth canal, mother pushes during contractions. Ends with the birth of the baby. Third Stage= Delivery of Placenta. The uterus continues to contract, placenta separates from uterine wall and is expelled through the vagina.*
Question 33:
**Answer: C) Prostate gland**
*Explanation: All the other structures are derived from mesonephric duct whilst prostate gland is derived from urogenital sinus.*
Question 34:
**Answer: C) Week 6
*Explanation: During embryonic development, the ureteric bud arises from the mesonephric duct and gives rise to the ureter, renal pelvis, calyces, and collecting ducts of the kidneys. Ureteric bud branching, which is essential for the formation of the collecting system of the kidneys, occurs around week 6 of embryonic development.
Question 35:
**Answer: C) Clitoris**
*Explanation: The clitoris contains erectile tissue and is responsible for sexual arousal and pleasure in females and is analogous to the male glans of penis.*
A is incorrect as labia majora is analogous to the scrotum in males since they are generated by labioscrotal swellings.
B is incorrect as labia minora is analogous to corpus spongiosum in males, since they are generated by urethral folds.
D is incorrect as it is analogous to the external urethral orifice in males.
E is incorrect as it is unique to female anatomy.
Question 36:
**Answer: C) Maintaining continence of feces**
*Explanation: The puborectalis muscle plays a crucial role in maintaining continence of feces by forming a sling-like structure around the rectum.*
Question 37:
**Answer: A) Inguinal canal**
*Explanation: The gubernaculum guides the testis through the inguinal canal as it descends into the scrotum during development.*
Question 38:
**Answer: C) Cremaster muscle**
*Explanation: The cremaster muscle surrounds the testes, helps regulate their temperature, and contracts to raise the testes closer to the body in response to external factors.*
A is incorrect as the epididymis is a coiled tube where sperm mature and are stored. It is located on the surface of the testis but does not regulate temperature or contract to move the testes.
B is incorrect as the dartos muscle is a smooth muscle in the scrotum that contracts in response to cold temperatures to reduce heat loss. It helps regulate the temperature of the testes by altering the surface area of the scrotum but does not directly surround the testes. Therefore, this is not the best answer.
D is incorrect as the tunica vaginalis is a serous membrane that covers the testis and provides a protective layer, but it does not contract or regulate temperature.
E is incorrect as vas deferens is a duct that carries sperm from the epididymis to the ejaculatory duct, but it does not regulate temperature or surround the testes.
Question 39:
**Answer: C) Seminal Vesicle**
Explanation: The seminal vesicle produces most of the seminal fluid (70%), including fructose and nutrients to support sperm function. D is incorrect as the prostate gland secretes a milky fluid that makes up a 1/3 of semen volume. Prostatic fluid contains enzymes, citric acid, and PSA (Prostate-Specific Antigen) that help liquefy semen and enhance sperm motility.
E is incorrect as the bulbourethral glands (Cowper’s glands) secrete a clear fluid that lubricates and neutralizes acidic conditions in the urethra during arousal. This fluid is released prior to ejaculation and does not contribute significantly to the overall ejaculate volume.*
Question 40:
**Answer: D) Hymen**
*Explanation: The hymen is a thin membrane that covers the vaginal opening and may be ruptured during first sexual intercourse or childbirth.*
** Question 41:**
**Answer: A) Pronephros**
*Explanation: The pronephros is the earliest kidney-like structure to appear during embryological development and is considered the most primitive.*
B is incorrect as the mesonephros is the second kidney-like structure to develop and functions as an temporary kidney during early embryonic development. It forms around the fifth week and is functional for a period before being replaced by the metanephros.
C is incorrect as the metanephros is the permanent kidney that forms later in development, around the fifth to sixth week. It develops from the ureteric bud and metanephric mesenchyme, eventually becoming the adult kidney.
D is incorrect as the nephron is the structural and functional unit of the kidney. It develops from the metanephric blastema and ureteric bud interaction during embryonic development.
E is incorrect as the ureteric bud is an outgrowth from the mesonephric duct that interacts with the metanephric mesenchyme to form the collecting ducts, renal pelvis, calyces, and ureters.
Question 42:
**Answer: C) Metanephros**
*Explanation: The metanephros is the final stage of kidney development, where functional nephrons are formed, and it becomes the definitive adult kidney. *
E is incorrect as the cloaca is an early embryonic cavity at the end of the hindgut where the digestive, urinary, and reproductive systems initially converge.
Question 43:
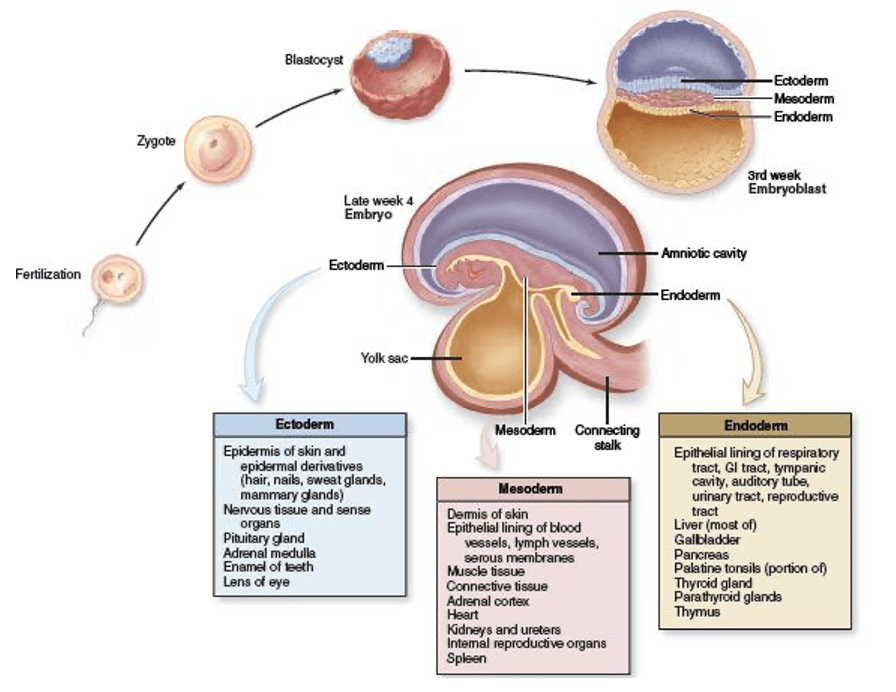
**Answer: B) Endoderm**
*Explanation: The urinary bladder has an endodermal origin, arising from the embryonic endoderm layer during development.*
Question 44:
**Answer: C) Mesoderm**
*Explanation: The mesoderm is the embryonic germ layer responsible for giving rise to the urogenital tract, including the kidneys, ureters, and reproductive organs.*
Question 45:
**Answer: C) Mesoderm**
*Explanation: The mesoderm is the embryonic germ layer responsible for giving rise to the urogenital tract, including the kidneys, ureters, and reproductive organs.*
Question 46:
**Answer: B) Gonadal ridge**
*Explanation: During early embryonic development, a pair of gonadal ridges develop along the posterior abdominal wall. These ridges give rise to the gonads, which are the testes in males and the ovaries in females. The differentiation into testes or ovaries depends on genetic and hormonal factors. Ovaries and testes are gonads, so they develop from the gonadal ridge.
A is incorrect as the urethra is a tubular structure that carries urine from the bladder to the outside of the body in both males and females. It does not give rise to the gonads.
C is incorrect as the wolffian duct is a precursor to parts of the male reproductive system, including the epididymis, vas deferens, and seminal vesicles. It does not give rise to the gonads.
D is incorrect as the mullerian duct is a precursor to parts of the female reproductive system, including the fallopian tubes, uterus, and upper part of the vagina. It does not give rise to the gonads.
E is incorrect as the cloaca is an early embryonic structure that forms as a common cavity where the digestive, urinary, and reproductive systems initially converge.
Question 47:
**Answer: A) Wolffian duct**
*Explanation: The Wolffian duct (aka mesonephric duct) is the precursor structure to the male internal genitalia, including the epididymis, vas deferens, and seminal vesicles, during embryonic development.*
Question 48:
**Answer: D) XO**
*Explanation: Individuals with Turner syndrome typically have a single X chromosome and no Y chromosome, denoted as XO. C is incorrect as XXY are the chromosomes for individuals with Kleinfelter’s syndrome.
A is incorrect as XX are the chromosomes for females
B is incorrect as XY are the chromosomes for males
C is incorrect as XXY are the chromosomes for male individuals with Kleinfelter’s syndrome
E is incorrect as XYY syndrome, are the chromosomes for male individuals with Jacobs syndrome.
Question 49:
**Answer: C) Filtration**
*Explanation: Filtration primarily occurs in the renal corpuscle, where blood is filtered to form the initial filtrate that will be processed further in the nephron.*
Question 50:
**Answer: C) To selectively return essential substances from the filtrate to the blood**
*Explanation: Tubular reabsorption in the kidney involves selectively reabsorbing essential substances (e.g., glucose, ions, water) from the filtrate back into the blood to maintain body homeostasis.*
Question 51:
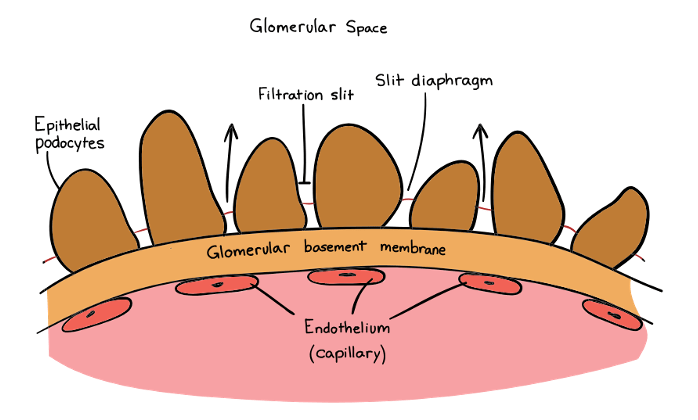
**Answer: C) To prevent blood cells and large proteins from entering the renal tubules**
*Explanation: The filtration membrane in the renal corpuscle acts as a selective barrier, allowing small molecules and ions to pass through while preventing the passage of blood cells and large proteins. It has three layers, an endothelial layer (simple squamous) that have small pores (fenestrae) allowing for the passage of small molecules and ions. These pores are large enough to permit the passage of substances like water, glucose, and electrolytes, but they restrict the passage of larger molecules such as blood cells and proteins. The next layer is the basement membrane and then podocytes which have finger-like projections called foot processes or pedicels that wrap around the capillaries of the glomerulus, all to prevent the movement of large molecules such as proteins into the tubules*
** Question 52:**
**Answer: D) Myogenic Autoregulation**
*Explanation: Myogenic Autoregulation of renal blood flow and GFR allows the kidneys to maintain relatively constant levels despite fluctuations in systemic blood pressure.*
A is incorrect as this is the process by which substances are actively transported from the blood into the renal tubules for excretion in urine. It is not related to the kidney’s ability to maintain renal blood flow and GFR.
B is incorrect as this is the process by which substances are reabsorbed from the renal tubules back into the bloodstream. While important for maintaining fluid and electrolyte balance, it is not specifically related to autoregulation of renal blood flow and GFR.
C is incorrect as this describes the regulation of osmotic pressure and water balance within the body. It involves processes like ADH secretion and water reabsorption in the kidneys, but it does not specifically describe the kidney’s ability to regulate blood flow and GFR in response to changes in blood pressure.
E is incorrect as this is the process by which fluid and solutes are filtered from the blood into the renal tubules at the glomerulus. While crucial for urine formation, it does not specifically describe the kidney’s ability to autoregulate blood flow and GFR.
Question 53:
Answer: B) GFR is the rate at which blood is filtered by the kidneys, and it is primarily regulated by autoregulation and hormonal mechanisms.
Explanation: GFR refers to the rate at which blood is filtered by the glomeruli of the kidneys. It measures the volume of fluid that filters into the kidney’s tubules per unit of time. GFR is primarily regulated by two main mechanisms: Autoregulation: This mechanism involves the ability of the kidneys to maintain a relatively constant GFR despite changes in systemic blood pressure. Autoregulation includes myogenic responses of the afferent arterioles and tubuloglomerular feedback mechanisms. Myogenic regulation refers to the ability of vascular smooth muscle cells in the walls of the afferent arterioles (and to some extent, the efferent arterioles) to respond to changes in blood pressure. When systemic blood pressure increases, the afferent arterioles constrict due to stretch-sensitive ion channels in the smooth muscle cells. This constriction helps maintain a relatively constant GFR by reducing blood flow into the glomerulus. Conversely, when blood pressure decreases, the arterioles dilate to maintain adequate blood flow and GFR. Tubuloglomerular feedback (TGF) is a mechanism by which the kidneys regulate glomerular filtration rate (GFR) based on the concentration of ions (especially sodium chloride) in the tubular fluid at the macula densa cells of the juxtaglomerular apparatus. When the GFR increases, more sodium reaches the macula densa cells in the distal convoluted tubule. This stimulates the macula densa cells to release adenosine, which constricts the afferent arteriole, reducing GFR. Conversely, a decrease in GFR results in less sodium reaching the macula densa cells, causing them to decrease adenosine release and dilate the afferent arteriole, increasing GFR. Hormonal Regulation involves hormones such as angiotensin II from the RAAS system, prostaglandins, and atrial natriuretic peptide (ANP), they play roles in regulating GFR by influencing renal blood flow and arteriolar resistance. For example, angiotensin II constricts the efferent arterioles to maintain GFR during low blood pressure states.
Question 54:
**Answer: E) To remove additional waste products and drugs from the blood into the urine**
*Explanation: Tubular secretion in the kidney involves the active transport of additional waste products and drugs from the blood into the urine for excretion.*
Question 55:
**Answer: D) Renal tubules**
*Explanation: The renal tubules are not part of the filtration membrane; they are located downstream from the renal corpuscle and are involved in further processing of the filtrate.*
Question 56:
**Answer: D) By the renin-angiotensin system to adjust GFR based on blood pressure**
*Explanation: The renin-angiotensin system is a hormonal mechanism that adjusts GFR based on changes in blood pressure by regulating blood vessel constriction and fluid balance.*
A is incorrect as ADH (vasopressin) primarily regulates water reabsorption in the collecting ducts of the nephron to control urine concentration, not GFR.
B is incorrect as ANP is released by the atria of the heart in response to increased blood volume and pressure. It promotes natriuresis (excretion of sodium in urine) and vasodilation to decrease blood volume and pressure, which would increase GFR rather than decrease it.
C is incorrect as aldosterone regulates sodium and water reabsorption in the distal tubules and collecting ducts of the nephron to maintain electrolyte balance and blood volume. It does not directly regulate GFR.
E is incorrect as insulin primarily regulates glucose metabolism and does not influence GFR.
Question 57:
The correct answer is D) Increased glucose levels, increased protein levels, increased water content.
Explanation: In diabetes mellitus, particularly in uncontrolled or poorly managed cases, alterations in urine composition can occur due to the inability of the kidneys to adequately reabsorb certain substances. The presence of glucose in the urine, known as glucosuria, is a hallmark feature of diabetes mellitus. Elevated blood glucose levels overwhelm the renal threshold for glucose reabsorption, leading to spillage of glucose into the urine. Additionally, diabetic nephropathy, a common complication of diabetes, can lead to proteinuria, the presence of excess proteins in the urine. This occurs due to damage to the glomeruli, the filtering units of the kidneys, resulting in leakage of proteins into the urine. As a result of increased glucose and protein levels in the urine, there is also increased water content, as both glucose and protein in the urine can draw water out of the body, contributing to polyuria (increased urination) and potential dehydration.
** Question 58:**
**Answer: B) Antidiuretic hormone (ADH)**
*Explanation: Antidiuretic hormone (ADH) regulates water reabsorption in the renal tubules, helping to concentrate or dilute urine based on body water needs whilst aldosterone works by increasing sodium reabsorption which bring water along with it.*
C is incorrect as aldosterone regulates sodium and potassium balance by increasing sodium reabsorption and potassium excretion in the distal convoluted tubule and collecting ducts. It indirectly affects water reabsorption by influencing sodium transport but is not primarily responsible for regulating water reabsorption. Therefore, this is not the best answer.
D is incorrect as ANP promotes natriuresis (sodium excretion) and vasodilation to reduce blood volume and pressure. It does not directly regulate water reabsorption in the renal tubules.
E is incorrect as Renin is an enzyme involved in the renin-angiotensin-aldosterone system, primarily regulating blood pressure and sodium balance. It does not directly regulate water reabsorption.
Question 59:
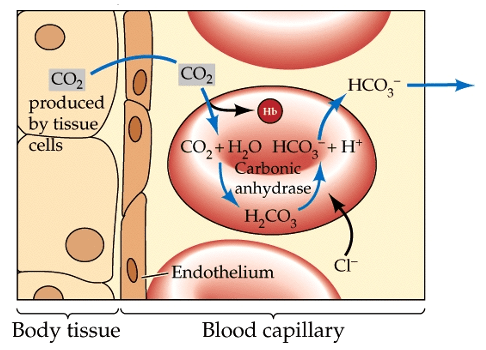
The correct answer is C) Chloride exchange with bicarbonate ions in red blood cells.
Explanation: During acid-base disturbances such as respiratory or metabolic acidosis, there is an increase in hydrogen ion (H+) concentration in the bloodstream. In response to this, chloride ions (Cl-) move into red blood cells from the plasma, facilitated by the anion exchange protein known as the chloride-bicarbonate exchanger (AE1 or Band 3 protein). Simultaneously, bicarbonate ions (HCO3-) move out of red blood cells into the plasma to buffer the excess H+ ions. This process is known as the chloride shift or Hamburger phenomenon. It helps to maintain electrochemical equilibrium across the red blood cell membrane and ensures efficient transport of CO2 from tissues to the lungs for elimination.
Question 60:
**Answer: A) To promote sodium reabsorption in the renal tubules**
*Explanation: Aldosterone regulates sodium and potassium balance by increasing sodium reabsorption and potassium excretion in the distal convoluted tubule and collecting ducts. It indirectly affects water reabsorption by influencing sodium transport due to osmosis, this leads to increased blood volume, which helps maintain fluid and electrolyte balance.*
Question 61:
**Answer: D) Atrial natriuretic peptide (ANP)**
*Explanation: ANP causes dilation to the afferent arteriole and constriction to the efferent arteriole in the kidneys, which increases glomerular filtration rate (GFR), enhances sodium excretion and inhibits its reabsorption in the collecting ducts. These actions help to reduce blood volume and pressure, counteracting the effects of high blood pressure and fluid retention.*
Question 62:
**Answer: C) Renal failure**
*Explanation: Renal failure can disrupt the kidney’s ability to regulate acid-base balance, potentially leading to acidosis.*
A is incorrect as hyperventilation can lead to respiratory alkalosis (not acidosis) by causing a decrease in carbon dioxide levels and an increase in blood pH.
B is incorrect as consumption of acidic foods does not typically lead to acidosis because the body has mechanisms to buffer and regulate blood pH.
D is partially incorrect as increased body temperature alone does not directly lead to acidosis. However, severe hyperthermia can lead to metabolic acidosis due to increased metabolic demands and tissue breakdown.
E is partially incorrect as dehydration can lead to a relative increase in blood acidity (acidaemia), but it does not typically cause true acidosis unless there are other underlying conditions affecting acid-base balance. Therefore, D and E are not the best answers.
Question 63:
Answer: C) Renin
Explanation: Renin is an enzyme secreted by the juxtaglomerular cells of the kidney in response to decreased blood pressure, low blood volume, or low sodium levels it acts to convert angiotensinogen, a protein produced by the liver, into angiotensin I, which is a precursor molecule in the Renin-Angiotensin-Aldosterone System (RAAS). Angiotensin I is subsequently converted to angiotensin II by the action of angiotensin-converting enzyme (ACE) primarily in the lungs. Angiotensin II is a potent vasoconstrictor and stimulates the release of aldosterone from the adrenal glands.
Question 64:
**Answer: C) To decrease blood volume and lower blood pressure**
*Explanation: ANP promotes the excretion of sodium and water in the urine, reducing blood volume and blood pressure, thus playing a role in fluid and electrolyte balance. ANP also achieves this by dilating blood vessels (vasodilation), which lowers blood pressure, inhibiting the renin-angiotensin-aldosterone system (RAAS), thereby reducing the effects of aldosterone and angiotensin II, both of which increase blood volume and pressure.*
Question 65:
**Answer: B) Creatinine clearance**
*Explanation: Creatinine clearance is a direct clinical measurement used to assess renal function by quantifying the volume of plasma from which creatinine is completely removed by the kidneys in a specified time period. Creatinine is a waste product of muscle metabolism that is freely filtered by the glomerulus and minimally reabsorbed or secreted by the renal tubules, making it a good indicator of glomerular filtration rate (GFR). Inulin is not used routinely and only in research, although it is the gold standard since it is completely filtered, not secreted or reabsorbed but the procedure is complex. PAH is a measure of renal plasma flow and not GFR.
Question 66:
**Answer: E) To stimulate red blood cell production in response to hypoxia**
*Explanation: Erythropoietin (EPO) is a hormone produced by the kidneys that stimulates the production of red blood cells in response to low oxygen levels (hypoxia) in the body.*
A is incorrect as this describes the function of RAAS system.
B is incorrect as this describes the function of angiotensin II.
C is incorrect as this describes the function of aldosterone.
D is incorrect as it is regulated by insulin and glucagon not EPO.
Question 67:
**Answer: D) Proteinuria**
*Explanation: Proteinuria is the presence of abnormal levels of protein in the urine and is often an indicator of renal disease or dysfunction.*
** Question 68:**
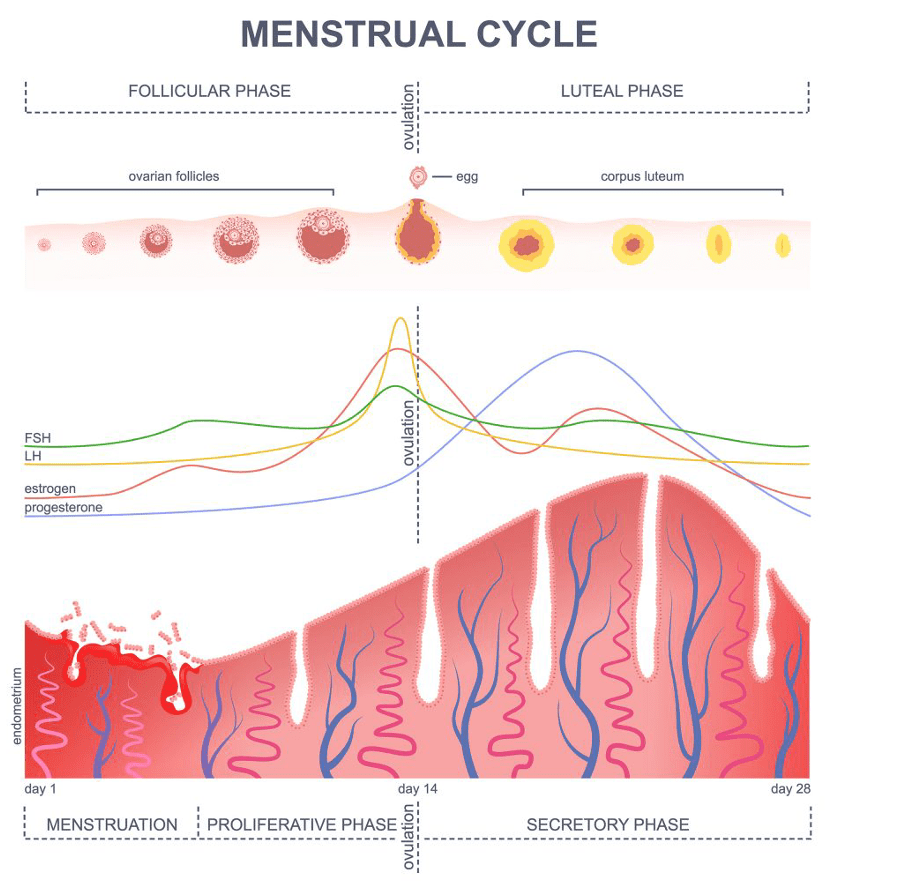
**Answer: A) Follicular phase**
Explanation: Menstrual Phase is the phase during which the uterine lining (endometrium) is shed, leading to menstruation. It marks the beginning of the follicular phase. Follicular Phase starts on the first day of menstruation and continues until ovulation. During the early part of the follicular phase, the uterine lining is shed, leading to menstruation.
B is incorrect as ovulation is the phase in which an egg is released from the ovary. It occurs midway through the menstrual cycle, around day 14 in a 28-day cycle under the influence of LH.
C is incorrect as the luteal phase follows ovulation and lasts until the start of menstruation. During the luteal phase, the endometrium is prepared for potential implantation of an embryo. If implantation does not occur, the corpus luteum degenerates, leading to a drop in progesterone and the onset of menstruation.
D is incorrect as the secretory phase (uterine cycle) is equivalent to the luteal phase (ovarian cycle) when the endometrium becomes more glandular and vascular in preparation for potential implantation.
E is incorrect as the proliferative phase (uterine cycle) is equivalent to the follicular phase (ovarian cycle), after menstruation has ended, and is characterised by the rebuilding of the endometrium under the influence of oestrogen.
Question 69:
**Answer: D) LH surge**
*Explanation: A surge in luteinizing hormone (LH) triggers the process of ovulation during the menstrual cycle.*
A is incorrect as oestrogen rises during the follicular phase and peak just before the LH surge. High oestrogen levels help to stimulate the LH surge but do not directly trigger ovulation.
B is incorrect as progesterone rises after ovulation during the luteal phase and helps maintain the uterine lining for potential implantation. It does not trigger ovulation.
C is incorrect FSH is important for the growth and maturation of ovarian follicles in the early part of the menstrual cycle. It peaks slightly before the LH surge but is not the primary trigger for ovulation.
E is incorrect hCG is produced by the placenta during pregnancy and is not involved in the ovulation process.
Question 70:
**Answer: C) Luteal phase**
*Explanation: The luteal phase is characterized by the formation of the corpus luteum which secrete progesterone. The rise in progesterone during the luteal phase helps to prepare the endometrium for potential implantation of a fertilized egg and maintains the uterine lining. *
Question 71:
**Answer: D) Progesterone**
*Explanation: Progesterone is responsible for maintaining the uterine lining (endometrium) during the luteal phase, making it suitable for potential implantation.*
Question 72:
**Answer: C) Oestrogen**
*Explanation: Oestrogen is the primary hormone responsible for thickening the uterine lining (endometrium) during the proliferative phase of the menstrual cycle.*
A is incorrect as LH is involved in triggering ovulation but does not directly influence the thickening of the endometrium during the proliferative phase.
B is incorrect as FSH stimulates the growth of ovarian follicles but is not the primary hormone responsible for the thickening of the endometrium.
D is incorrect as progesterone is involved in maintaining the endometrium and preparing it for implantation during the luteal phase but does not play a significant role in thickening the endometrium during the proliferative phase.
E is incorrect as hCG is produced by the placenta during pregnancy and is not involved in the menstrual cycle phases leading up to ovulation.
Question 73:
**Answer: C) Atrial septal defect (ASD)**
*Explanation: Atrial septal defect (ASD) is a congenital heart defect characterized by a hole in the septum between the heart’s two upper chambers.*
Question 74:
**Answer: A) Luteinizing hormone (LH)**
*Explanation: LH is responsible for stimulating the Leydig cells in the testes to produce testosterone in the male reproductive system.* LH = Leydig cells. FSH = Sertoli cells.
Question 75:
**Answer: E) Progesterone**
*Explanation: Progesterone, primarily secreted by the placenta, helps maintain pregnancy by preventing uterine contractions and supporting the uterine lining during the first trimester. The answer is not hCG as although hCG does play a role in supporting the corpus luteum to continue producing progesterone until the placenta takes over its production, progesterone itself is directly responsible for preventing uterine contractions and supporting the uterine lining in the first trimester until the placenta is able to take over this function.*
Question 76:
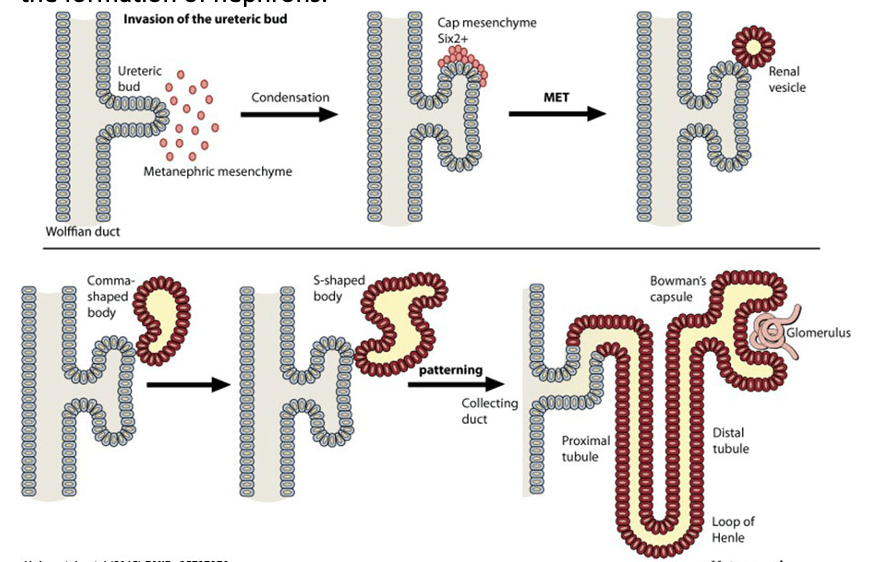
Answer: b) Reciprocal induction
Explanation: Reciprocal induction refers to the mutual signalling between the ureteric bud and the metanephric blastema, which is crucial for the differentiation and development of kidney structures. The ureteric bud secretes growth factors that induce the metanephric blastema to form nephrons, and the metanephric blastema secretes factors that promote branching and development of the ureteric bud.
a) is incorrect as paramesonephric duct signalling is involved in the development of the female reproductive system and not nephron formation.
c) is incorrect as mesonephric duct apoptosis is related to the regression of the mesonephric duct in females but not nephron development.
d) is incorrect as pronephros degeneration involves the pronephros, which is an early, transient kidney structure that degenerates and is not directly involved in nephron formation.
e) is incorrect as wolffian duct differentiation is a process that contributes to the development of male reproductive structures and does not directly involve the formation of nephrons.
Question 77:
Answer: c) Metanephric blastema
Explanation: Metanephric blastema is the tissue that differentiates into nephrons, including the renal corpuscle and various segments of the nephron.
a) is incorrect as the pronephros is an early, transient structure in kidney development that regresses and does not form part of the definitive kidney.
b) is incorrect as the mesonephros is an intermediate kidney and is partially functional during early development but does not contribute to the permanent kidney structures.
d) is incorrect as the ureteric bud gives rise to the collecting ducts, calyces, renal pelvis, and ureters, but not the nephron itself.
e) is incorrect as the paramesonephric duct is involved in the development of the female reproductive system, not the kidney.
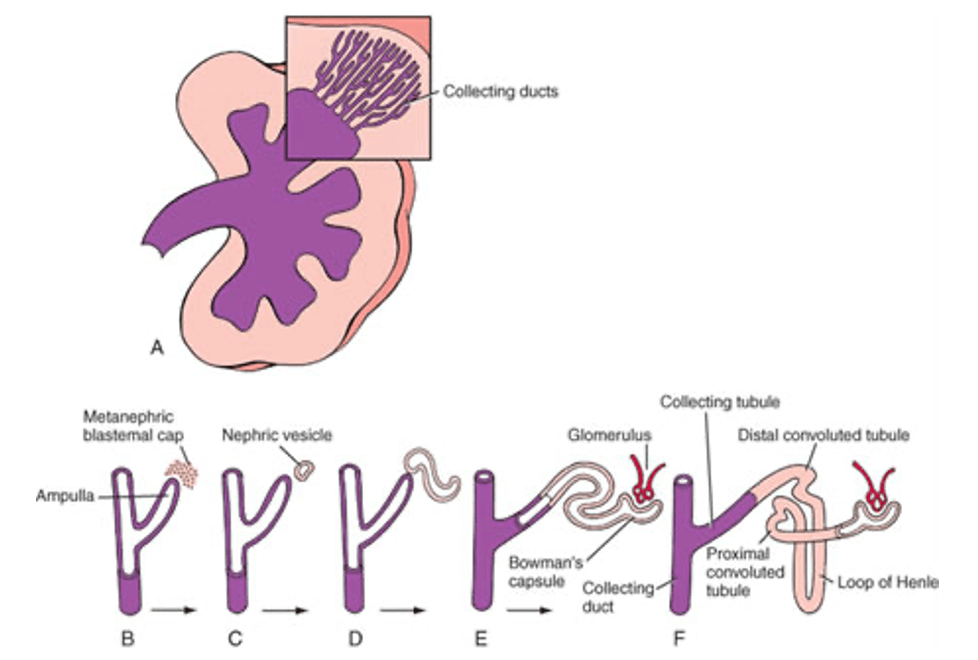
Question 78:
Answer: c) Glomerulus
Explanation: the glomerulus, which is part of the renal corpuscle nephron located in the renal cortex where blood filtration begins.
a) is incorrect as the Loop of Henle extends into the medulla.
b) is incorrect as the collecting ducts extend from the cortex through the medulla.
d) is incorrect as the renal pelvis is in the renal sinus and collects urine from the major calyces.
e) is incorrect as minor calyces are found in the renal sinus, not the cortex.
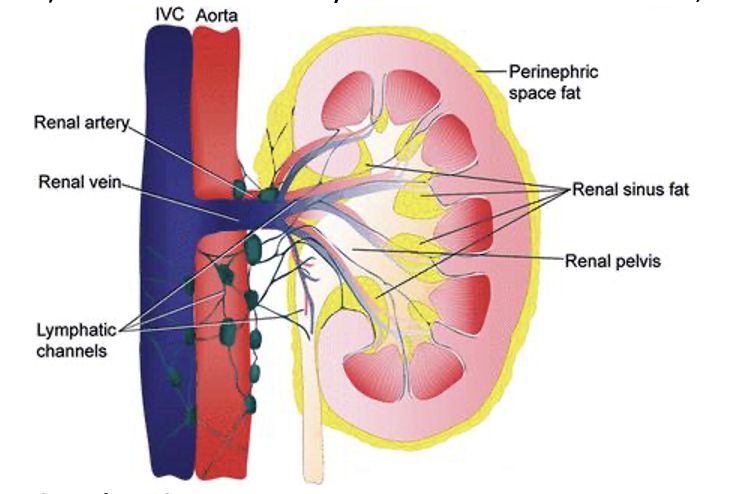
Question 79:
Answer: c) Between the 12th thoracic and 3rd lumbar vertebrae
Explanation: the 12th thoracic and 3rd lumbar vertebrae is the typical position of the kidneys, with the right kidney slightly lower than the left due to the presence of the liver.
a) is incorrect as this location is too high and is not where the kidneys are found.
b) is incorrect as this location is slightly lower than the actual position.
d) is incorrect as this location is too high for the kidneys.
e) is incorrect as this location is slightly lower than the actual position.
Question 80:
Answer: b) Ureteropelvic junction, crossing over the iliac vessels, and ureterovesical junction
Explanation: Ureteropelvic junction, crossing over the iliac vessels, and ureterovesical junction are the three common constriction points where kidney stones may become lodged.
a) is incorrect as the iliac crest is not a constriction point.
c) is incorrect as the renal cortex is not a ureteral constriction point.
d) is incorrect as the renal medulla and iliac crest are not constriction points.
e) is incorrect as the renal pelvis is not a constriction point.
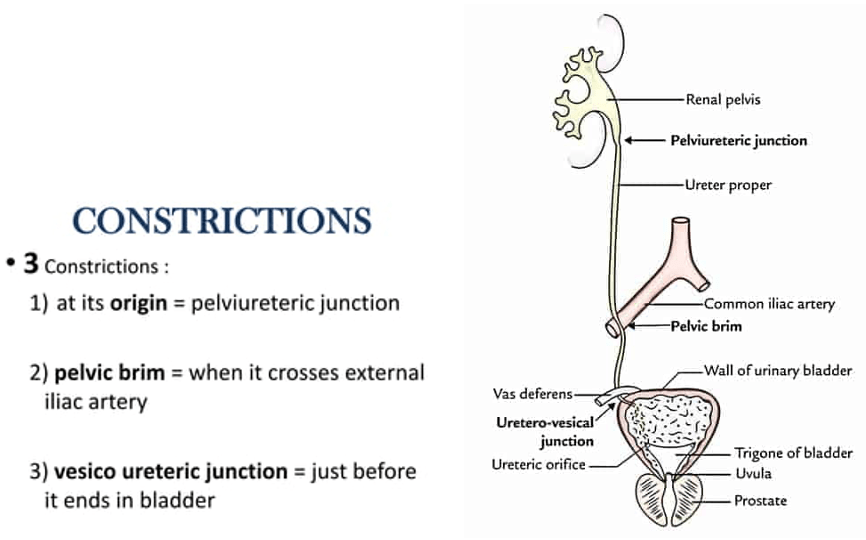
Question 81:
Answer: d) Transitional epithelium
Explanation: transitional epithelium, lines the bladder and allows it to stretch and expand.
a) is incorrect as simple squamous epithelium is too thin for the bladder’s needs and is found in structures like the alveoli of the lungs.
b) is incorrect as stratified squamous epithelium is found in areas subject to abrasion, like the skin and oesophagus, not the bladder.
c) is incorrect as simple cuboidal epithelium is found in glands and ducts, not the bladder.
e) is incorrect as pseudostratified columnar epithelium is found in the respiratory tract such as the trachea, not the bladder.
Question 82:
Answer: c) Pelvic splanchnic nerves
Explanation: the pelvic splanchnic nerves, carry parasympathetic fibres that control bladder contraction and the sensation of fullness.
a) is incorrect as the sciatic nerve innervates the (posterior) lower limb and is not involved in bladder control.
b) is incorrect as the hypogastric nerve carries sympathetic fibres involved in bladder relaxation, but it is not the primary nerve for sensation and motor control.
d) is incorrect as the femoral nerve innervates the anterior thigh muscles and is not involved in bladder control.
e) is incorrect as the phrenic nerve innervates the external urethral sphincter not the bladder.
Question 83:
Answer: a) Renal vein, renal artery, ureter
Explanation: The correct order is from anterior to posterior, with the renal vein being the most anterior, followed by the renal artery, and the ureter being the most posterior.
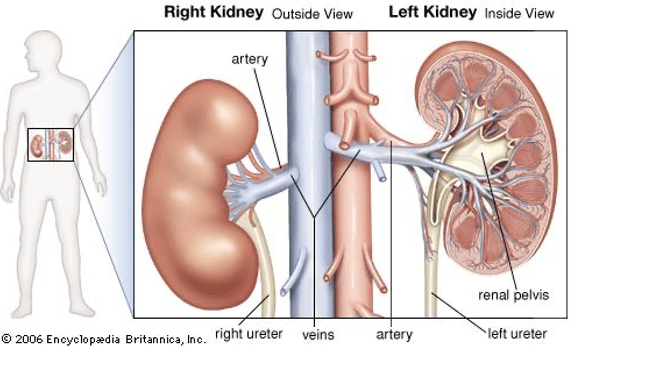
Question 84:
Answer: a) Detrusor muscle
Explanation: the detrusor muscle, a smooth muscle that contracts to expel urine from the bladder.
b) is incorrect as the dartos muscle is found in the scrotum and is involved in the regulation of scrotal temperature.
c) is incorrect as the cremaster muscle is also found in the scrotum and helps to control the position of the testes in order to maintain optimum temperatures for spermatogenesis.
d) is incorrect as the external urethral sphincter is a muscle that controls the release of urine but does not expel it.
e) is incorrect as the internal urethral sphincter controls the flow of urine into the urethra but does not expel it, it does this by relaxing to allow urine to enter the urethra not by contracting.
Question 85:
Answer: b) Fenestrated endothelium, basement membrane, podocytes
Explanation: the fenestrated endothelium of the glomerular capillaries, the glomerular basement membrane, and the podocytes (visceral epithelial cells) which form the filtration slits.
c) is incorrect as transitional epithelium is found in the bladder, not the renal corpuscle.
d) is incorrect as cuboidal epithelium is found in renal tubules, not the renal corpuscle.
Question 86:
Answer: d) In the walls of the afferent arteriole
Explanation: the juxtaglomerular cells are located in the walls of the afferent arteriole, where they secrete renin.
a) is generally true but is not specific enough.
c) is incorrect as they are specifically located in the afferent arteriole walls, not directly around the capillaries.
e) is incorrect as the distal convoluted tubule is where the macula densa is located, not the juxtaglomerular cells.
Question 87:
Answer: c) To sense sodium concentration in the distal convoluted tubule
Explanation: the macula densa cells detect sodium concentration in the DCT, which influences the release of renin by juxtaglomerular cells. If the concentration of sodium is low it indicates that the GFR and blood pressure is low, hence juxtaglomerular cells secrete renin which participates in the RAAS system to increase BP and GFR.
a) is incorrect as this function is primarily carried out by cells in the PCT and other nephron segments such as DCT. Aldosterone further aids in the reabsorption of sodium in the DCT but this is initially triggered by macula densa cells that detect a decrease in sodium concentration.
b) is incorrect as this is the role of juxtaglomerular cells, not macula densa cells.
d) is incorrect as this function is carried out by interstitial cells of the peritubular capillaries in the kidney, not the macula densa.
e) is incorrect as this is the role of the glomerulus, not the macula densa.
Question 88:
Answer: a) The volume of plasma filtered per minute by all nephrons in the kidneys
Explanation: GFR measures the rate at which blood is filtered in the glomeruli of the kidneys.
b) is incorrect as this describes urine flow rate or urine output, which measures the amount of urine produced by the kidneys and delivered to the bladder, not GFR.
c) is incorrect as it describes renal blood flow (RBF), which is the volume of blood delivered to the kidneys per unit time, not the GFR.
d) is incorrect as it describes the renal tubular reabsorption rate for sodium, which is the amount of sodium reabsorbed in the PCT, not the GFR.
e) is incorrect as it describes urea excretion rate or urea clearance, which measures how much urea is removed from the blood and excreted in the urine, not the GFR.
Question 89:
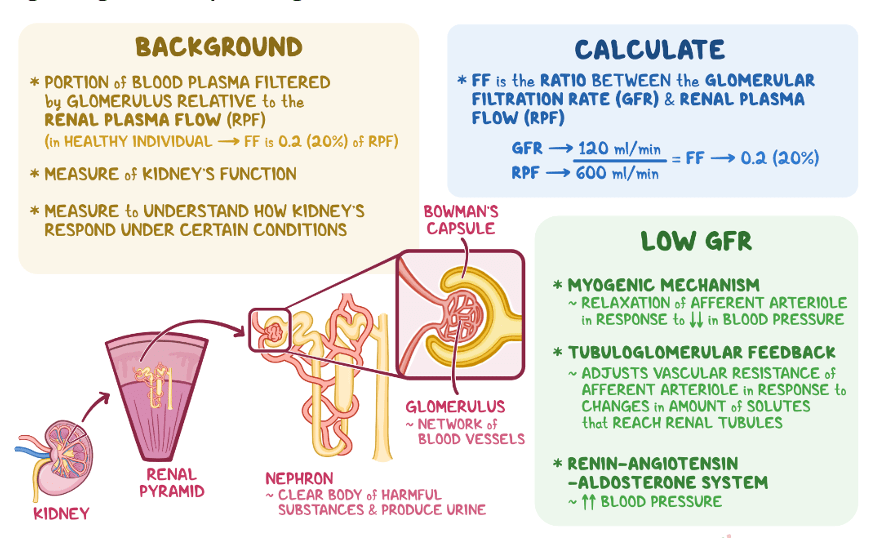
Answer: b) 20%
Explanation: the filtration fraction, is the ratio of GFR to renal plasma flow, and is normally about 20% in healthy adults. GFR above 50% indicates the beginning of kidney damage.
Question 90:
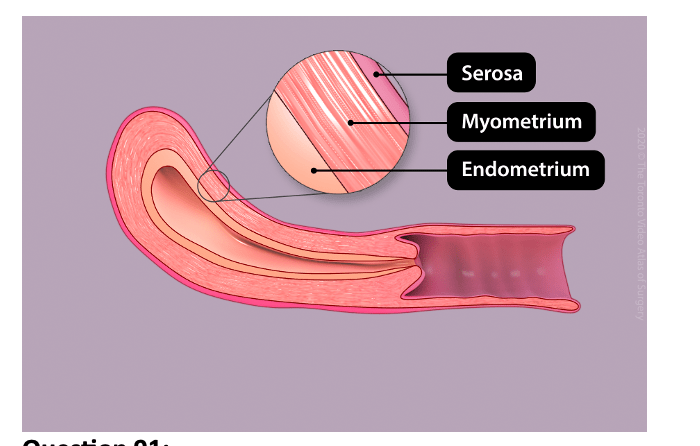
Answer: a) Endometrium, myometrium, perimetrium
Explanation: the correct order from innermost to outermost: the endometrium is the inner lining made from unkeratinised stratified simple squamous epithelium, the myometrium is the thick muscular layer, and the perimetrium is the outer serous layer.
Question 91:
Which of the following structures is homologous to the male penis?
Answer: b) Clitoris
Explanation: the clitoris, is homologous to the male penis as both develop from the genital tubercle which turns into the phallus and differentiates into either clitoris or penis depending on the presence of the SRY gene which causes the mesonephric (wolffian) duct to secrete testosterone from leydig cells that is later converted to DHT by 5 alpha reductase and stimulates the formation of male external genitalia. Absence of SRY gene means that the mesonephric duct regresses due to the absence of testosterone and clitoris develops from the paramesonephric duct to increased oestrogen.
a) is incorrect as labia majora are homologous to the scrotum in males.
c) is incorrect as urethral folds develop into the penile urethra in males or the labia minora in females.
d) is incorrect as labia minora in females is homologous penile urethra in males.
e) is incorrect as Bartholin’s glands (greater vestibular glands) are homologous to Cowper’s glands (bulbourethral glands) in males.
Question 92:
Answer: a) Becomes the scrotal ligament in males and the round ligament in females
Question 93:
Answer: e) Oestrogen, produced by the granulosa cells
Explanation: oestrogen, is produced by the granulosa cells and is responsible for the positive feedback mechanism that triggers the LH surge during ovulation due to the lack of progesterone.
a) is incorrect as LH is produced by the anterior pituitary.
b) is incorrect as theca interna cells produce androgens, which are converted to oestrogen in granulosa cells by aromatase.
c) is incorrect as progesterone is involved the negative feedback, not in the positive feedback for ovulation.
d) is incorrect as while LH is involved in ovulation, it is not responsible for the positive feedback mechanism.
Question 94:
Answer: b) Leydig cells, located in the interstitial tissue of the testes
Explanation: Leydig cells, produce testosterone and are located in the interstitial tissue of the testes between the seminiferous tubules.
a) is incorrect as Sertoli cells support spermatogenesis but do not produce testosterone.
c) is incorrect as spermatogonia are germ cells that develop into spermatozoa, not hormone-producing cells.
d) is incorrect as granulosa cells are found in the ovarian follicles, not in the testes and they produce oestrogens not testosterone.
e) is incorrect as theca cells are found in the ovaries, not in the testes.
Question 95:
Answer: b) Spermiogenesis
Explanation: spermiogenesis, is the process of transforming spermatids into mature spermatozoa.
a) is incorrect as spermatogenesis is the overall process of sperm production, including spermiogenesis.
c) is incorrect as spermiation is the release of mature spermatozoa into the lumen of the seminiferous tubules, through the straight tubules, into the rete testis, into the efferent ductules head and tail of epididymis and the vas deferens.
d) is incorrect as oogenesis is the process of egg (ovum) development in females.
e) is incorrect as folliculogenesis is the development of ovarian follicles in females.
Question 96:
Answer: a) Gravidity 4, Parity 2
Explanation: Gravidity 4 (total number of pregnancies, including the current one) and Parity 2 (number of pregnancies that are past 20 weeks regardless of whether of the outcome). She is currently pregnant, making her gravidity 4, and her parity is 2 due to the two full-term deliveries- have gone past 20 weeks.
b) Gravidity 3, Parity 2 is incorrect gravidity as she has had four pregnancies including the current one.
c) Gravidity 4, Parity 3 is incorrect parity as she has had two full-term deliveries, the abortion was at 8 weeks, it needs to be past 20 weeks to be considered parity 3.
d) Gravidity 3, Parity 3 is Incorrect gravidity and parity as she has had four pregnancies, and one of her pregnancies did not surpass 20 weeks.
e) Gravidity 4, Parity 1 is incorrect parity as she has had two full-term deliveries.

Question 97:
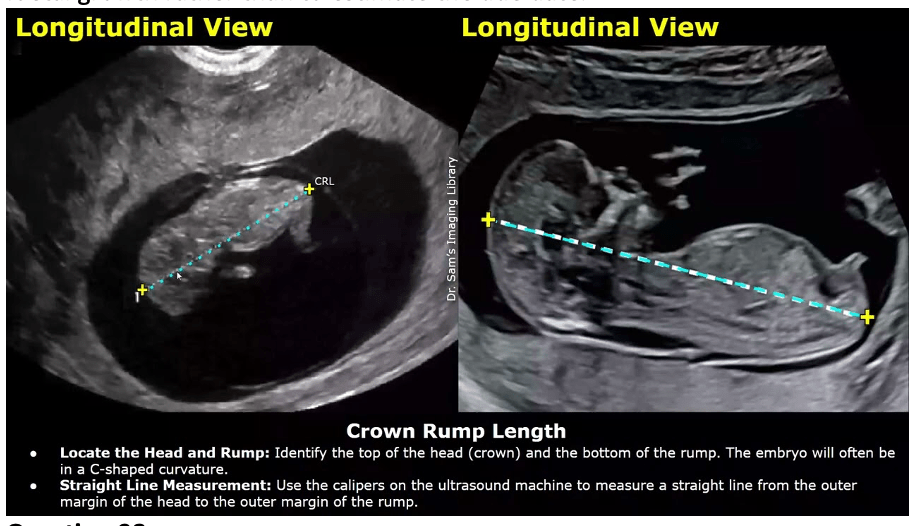
Answer: b) Gestational age based on ultrasound measurement of crown-rump length (CRL)
Explanation: Measurement of CRL via ultrasound is the most accurate method for estimating the due date, especially in the first trimester, due to its precision. The CRL method involves measuring the length of the foetus from the crown of the head to the rump (buttocks) during an early ultrasound (usually in the first trimester). This measurement is used to estimate gestational age.
a) is incorrect as the Last menstrual period (LMP) method is influenced by irregular menstrual cycles making it less reliable. The LMP method is a common approach where the due date is calculated based on the first day of the woman’s last menstrual period. The standard calculation is: subtract 3 months from the first day of a woman’s period and add 7 days to it.
c) is incorrect as calculation based on conception date is influenced by the exact date of conception, the exact date of conception is often unknown, which can lead to inaccuracies.
d) is incorrect as this method involves estimating the gestational age from the date when a pregnancy test first turns positive but is less precise because it doesn’t provide a clear gestational age and is influenced by hormone levels that vary between individuals.
e) is incorrect as estimation based on maternal fundal height, varies with maternal weight. It involves assessing the distance from the pubic symphysis to the top of the uterus (fundus). This measurement is typically used to track foetal growth rather than to estimate the due date.
Question 98:
Answer: a) FF = GFR / RPF, where FF represents the fraction of plasma filtered
Explanation: Filtration Fraction (FF) is calculated as GFR divided by RPF, representing the proportion of plasma that is filtered.
Question 99:
Answer: b) The female pelvic inlet is wider and more circular, compared to the male pelvic inlet.
Explanation: The female pelvic inlet is broader and more circular to accommodate childbirth, whereas the male pelvic inlet is narrower and more heart-shaped.
Question 100:
Answer: d) The cremaster muscle elevates the testis and is innervated by the genitofemoral nerve.
Explanation: The cremaster muscle helps in elevating the testis and is innervated by the genital branch of the genitofemoral nerve. In colder temperatures, the cremaster muscle contracts to pull the testis closer to the body, thereby warming it. This helps to maintain the temperature necessary for optimal sperm production. Conversely, in warmer conditions, the muscle relaxes to lower the testis further from the body, allowing it to cool down.
a) is incorrect as while the cremaster muscle does elevate the testis, it is not innervated by the ilioinguinal nerve. The ilioinguinal nerve innervates the skin over the groin and the base of the penis but not the cremaster muscle.
b) is incorrect as pelvic splanchnic nerves innervate the parasympathetic portion of the bladder not the cremaster muscle.
c) is incorrect as although the cremaster muscle does assist in thermoregulation, it is innervated by the genitofemoral nerve, not the iliohypogastric nerve, which primarily provides sensory innervation to the skin of the lower abdomen.
e) is incorrect as the cremaster muscle is not involved in penile erection; this function is related to other muscles (such as corpus cavernosum) and is innervated by the pudendal nerve, which also does not innervate the cremaster muscle.
Question 101:
Answer: c) Ischiocavernosus
Explanation: The ischiocavernosus muscle is involved in penile erection in males and clitoral erection in females but does not play a role in supporting the pelvic floor.
a) is incorrect as the levator ani is a major muscle group (consisting of iliococcygeus and pubococcygeus and sometimes puborectalis) in the pelvic floor, providing support to pelvic organs.
b) is incorrect as the coccygeus muscle supports the pelvic floor and helps maintain the position of the pelvic organs alongside levator ani.
d) is incorrect as the pubococcygeus muscle is a part of the levator ani group, supports the pelvic floor and helps maintain continence.
e) is incorrect as the puborectalis muscle, also part of the levator ani group, supports the pelvic floor and maintains faecal continence.
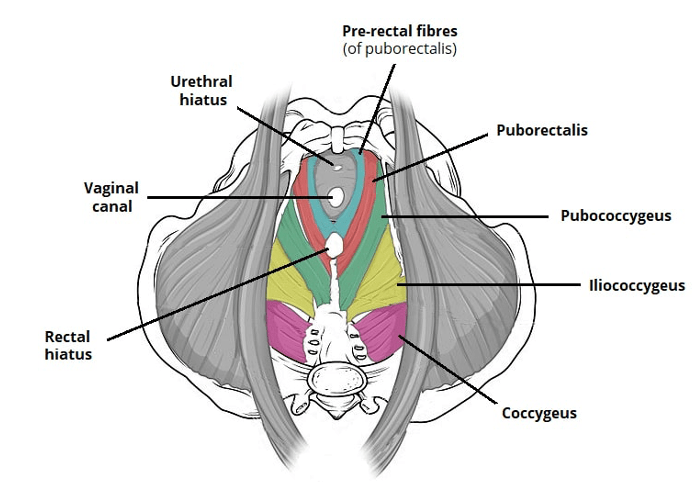
Question 102:
Answer: a) Compressor urethrae
Explanation: The compressor urethrae muscle provides voluntary control over the external urethral sphincter, helping to prevent urinary leakage during activities that increase abdominal pressure.
b) is incorrect as sphincter urethrovaginalis is a muscle that surrounds both the urethra and vagina but is not the primary muscle responsible for the external urethral sphincter control.
c) is incorrect as pubococcygeus muscle is part of the levator ani group that supports the pelvic floor but is not specifically responsible for external urethral sphincter control.
d) is incorrect as ischiocavernosus muscle is involved in penile and clitoral erection but does not control the external urethral sphincter.
e) is incorrect as bulbospongiosus muscle aids in penile erection and ejaculation but does not control the external urethral sphincter.
Question 103:
Answer: c) Seminal vesicles
Explanation: The seminal vesicles produce a significant portion of seminal fluid, which provides nutrients, a medium for sperm transport, and helps to neutralise vaginal acidity.
a) is incorrect as the prostate gland produces a milky fluid that also contributes to semen but is not the primary source of seminal fluid, it contributes to 25% of all seminal fluid.
b) is incorrect as bulbourethral glands (Cowper’s glands) produce a pre-ejaculatory fluid that helps lubricate the urethra but is not the main contributor to seminal fluid.
d) is incorrect as the epididymis stores and matures sperm but does not produce seminal fluid.
e) is incorrect as the vas deferens transports sperm but does not produce seminal fluid.
